
The Bikini Hip Replacement - Surgical Technique Preserving Vessels and Deep Soft Tissues in Direct Anterior Approach Hip Replacement
*Corresponding Author(s):
Ikram NizamSpecialist Orthopaedic Surgeon, Ozorthopaedics, 1356 High Street Malvern, VIC 3144, Melbourne, Australia
Tel:+61 398884938,
Fax:+61 398807768
Email:info@ozorthopaedics.com.au
Abstract
We provide a single surgeon experience of 100 cases describing the technique of directing anterior approach to the hip through a bikini incision (bikini hip replacement) without a traction table preserving the branches of the external circumflex lateral vessels, antero-medial capsule and adjacent labrum with limited dissection of the tensor fascia-lata.
At an average of 17.2 months (7.1 to 24.1), we found no evidence of groin pain or residual numbness in the lateral thigh. 1 patient had a haematoma due to increased anticoagulation that resolved spontaneously. All components were well placed with no dislocations or leg length discrepancies until the most recent follow up.
In conclusion, this soft tissue sparing technique using the bikini incision direct anterior approach is safe and led to no incidence of groin pain or lateral thigh numbness at the most recent follow-up.
Keywords
Anterior approach; Bikini hip replacement; Muscle sparing
INTRODUCTION
The anterior hip arthroplasty has claimed less damage to muscles [4-6] and quicker recovery with less pain and early independent ambulation with improved gait [7-10].
Although most of the Direct Anterior Approaches (DAA) have performed through a longitudinal incision, Leunig et al., [11] reported hip arthroplasties through a bikini line incision with improved scar appearance in relatively thinner patients compared to longitudinal incisions [10].
An increased risk of bleeding has been reported with the DAAs compared to the conventional posterolateral approach [12] with parasthesia reported in up to 14.8-81% with a decrease in symptoms overtime [13,14].
The aim of this surgical approach was to determine if the author’s soft tissue sparing surgical technique reduced the incidence of groin pain and paraesthesia in the bikini total hip replacements with less incidence of haematoma formation by preserving the lateral circumflex vessels.
MATERIALS AND METHODS
During the follow-up periods, patients were specifically asked for any post-operative groin pain or discomfort and lateral thigh numbness. Clinically, they were assessed for haematoma formation in the operative site and anterolateral thigh for up to 8 weeks.
SURGICAL TECHNIQUE
Operating table and patient positioning
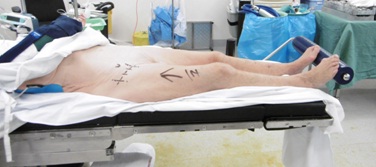
Landmarks and incision
Perioperative prophylactic antibiotics were given before and after surgery (IV Cefuroxime 2g). If required a longitudinal incision can be made in the form of a “T” incision from the bikini incision downwards and distal if difficult cases are encountered or extensive intraoperative fractures. We did not encounter any such cases. Patients should be informed this at all times during surgical consent.
Superficial and deep dissection
A longitudinal incision was made in the TFL approximately 3 cm below and lateral to the ASIS and the medial flap elevated utilizing the subfascial plane between the TFL and Sartorius. The TFL dissection only passed just 2-3 cm below the lateral circumflex vessels to protect the lateral branches of the lateral femoral cutaneous nerve. The ascending branches of the lateral circumflex iliac vessels were identified and preserved (Figure 2). The reflected head of rectus was gently teased off the capsule with a cob elevator and special retractors were then placed on the medial and lateral femoral neck outside the capsule (Figure 2).
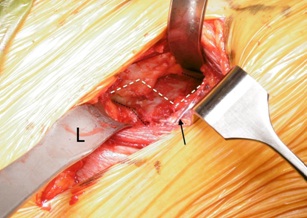
Figure 2: Arrow showing preservation of the lateral circumflex branches and capsule exposed with medial and Lateral (L) retractors. The black dotted line - femoral neck outline. The white line depicts the “Z” Capsulotomy that was performed in a right hip.
Capsulotomy and femoral preparation
A neck osteotomy was performed at the predetermined level. A further osteotomy was performed 5mm more proximal to remove a wedge of neck (napkin ring) enabling easy extraction of the head.
Only a small portion of the supero-lateral capsule was dissected and removed. The posterolateral capsule adjacent to the external rotators was carefully reflected from the neck with the aid of a large bone hook just enough to deliver the proximal femur for broaching (Figure 3) and the leg placed in figure 4. The femur was prepared first as a surgeon preference with the operated leg in a figure 4, position and the table broken to 45 degrees.
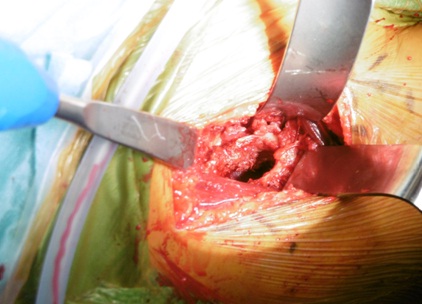
Figure 3: Femoral preparation after postero-lateral capsular release and femur exposed with femoral elevator (blue handle) with leg in figure 4, position.
The femur was broached with a woodpecker attached to a double offset handle to the templated size making sure the modular broach was not in varus and left in situ.
Acetabular preparation
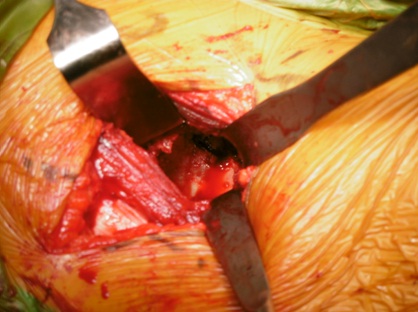
Figure 4: Acetabular exposure with careful placement of infero medial and infero lateral retractors (Right Hip). The infero medial retractor at 5’0 clock position-below the transverse ligament and infero lateral retractor at 8’0 clock position of acetabular margins in a right hip.
The acetabulum was reamed in increments with a double offset reamer and trialled before introducing the definitive component making sure the cup was positioned at approximately 40 degrees inclination and 15-20 degree anteversion with a double offset cup introducer. Adequate seating of the cup was assessed with a depth gauge through the screw holes. No intra operative X-rays were performed in any of the procedures. 2 screws were placed in all cases. The edge of the cup on the medial aspect was well covered with bone or thick capsule in all cases protecting the iliopsoas tendon infront. A 20 degree hooded liner was then introduced and impacted with the hood apex placed supero-laterally. Trial reductions were carried out before definitive stem was introduced and re-trialled with head sizes and leg lengths easily measured at the end of the table by feeling the medial malleoli ensuring the pelvis was square.
Components
Stability testing
Local infiltration analgesia was carried out as per Kerr-Kohan in all cases as a part of our rapid recovery programme [15]. The lateral circumflex vessels were always protected and checked for integrity (Figure 5).
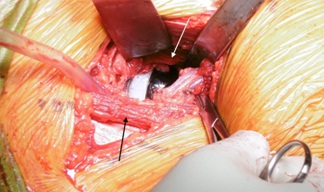
Figure 5: Lateral Circumflex vessel branches still intact after components inserted before wound closure. Antero medial capsule preserved (light arrow). The TFL still preserved at the end (dark arrow).
No wound drains were used in any patients.
The surgical times ranged from 48minutes to 135minutes (average 79mins).
Post-operative care
RESULTS
| Diagnosis | |
| Osteoarthritis | 98 |
| Fracture NOF* | 2 |
| Age | 67 yrs (49 to 86) |
| Sex | F=58, M=37 |
| BMI | 27.9 (23.1 to 34.8) |
| Follow-up | 7.2 months (4.1 to 18.1) |
The majority (71%) were discharged within the first 24-48 hours post surgery enabled by our enhanced recovery programme. The rest were living home alone and waited longer for a rehabilitation bed. Most patients who went home were driving a car at an average of 11 days (3 days to 29 days).
There were no signs of superficial or deep infection or haematoma formation at early follow-up except in 1 patient who had been inadvertently taking both aspirin 300mg daily and 40mg subcutaneously. This was detected and stopped immediately at day 12 post-op. The haematoma resolved without surgical intervention. There were no dislocations or leg length discrepancies (clinical or radiological). Post operative X-rays revealed well placed acetabular and femoral components in all cases.
Until the most recent follow up no patient complained of groin pain. 2 patients had reduced sensation over the LFCN distribution which resolved with time over 26 weeks.
Intraoperatively, 1 patient had a hairline fracture only extending to the lesser trochanter but not beyond. A standard non-offset broach was being used at the time as the double offset broach was unavailable for that case. This small fracture was cerclage wired although post operatively the stem was solidly fixed with no evidence of fracture propagation. The wire was removed 8 weeks later as it was irritating the tensor fascia lata.
Another patient had a fall 3 weeks post surgery sustaining a periprosthetic fracture which was revised to a cemented long stem and fixation of fracture through posterior approach. At the most recent follow up, the components were well placed and integrated.
DISCUSSION
Emphasis should be extended to what happens under the skin incision, since this is more important than the length of the scar itself. What matters ultimately is component positioning without complications to reduce dislocations and improve longevity and function.
Leunig et al., [10] described the bikini incision for anterior approaches to the hip as it followed the anatomic cleavage lines (Langers lines) with better scars as opposed to the longitudinal scars in the standard DAA. The author of this paper was fortunate and thankful to see this incision and technique by Leunig and modify the dissection in the deeper layers with the ability to do the procedure with only 1 assistant. The author of this paper had the same experience where bikini incisions had improved scars and aesthetic appearance compared to longitudinal incisions. Our center is in the process of comparing a larger number of our longitudinal vs bikini incisions performed by a single surgeon.
The soft tissue in the path to the actual hip joint itself should be preserved as much as possible as every part handled, dissected or cut would lead to local trauma, bleeding, swelling and this would in-turn result in pain and relative limitation of function slowing recovery.
The standard DAA approaches still involve extensive dissection with ligation/cautery of the LFCA branches, extensive dissection of capsule and removal of labrum. Our technique is minimally invasive but maximally preserving with limited dissection of soft tissue and lateral circumflex vessel preservation and preserving the antero-medial capsule and adjacent labral tissue underneath. If the labrum interfered with cup seating some lateral labrum can be removed. This is because the 2 soft tissue layers can protect the anterior flexors from any irritation and subsequent pain. We did not have a single case with groin pain at the most recent follow up.
Unlike the standard DAA approaches, we preserved the branches of the lateral circumflex because even if these vessels were cauterized or ligated, with subsequent retraction and/or cessation of the temporary vasospasm (especially after cautery), these vessels may re-bleed after the wound is closed and present as haematoma or thigh swelling. This may in-turn slow recovery. In our approach described we did not need to interfere with the vessel as we managed to have good access to the proximal femur with the lateral circumflex vessels preserved.
The bikini incision anterior hip replacements were initially offered to patients with less fat and muscle over the anterior thigh. However with time the surgeon was more comfortable to extend this to patients with up to 132kg body weight.
The Lateral Femoral Cutaneous Nerve (LFCN) is at risk irrespective of the approach be it longitudinal or bikini incision. It is the deep soft tissue dissection that will determine if the nerve is at risk. Any aggressive medial retraction or extension of the TFL splitting further than 2-3centimeters beyond the level of the lateral circumflex vessels can endanger the branches of the LFCN resulting in thigh numbness. This was another reason why the lateral circumflex vessels were preserved as it acted as a landmark avoiding extensive distal TFL splitting.
The author preferred the non-traction table approach as it was much easier to check leg lengths and stability and reduced preparation time and patient change over times. This will certainly vary among surgeons and they should choose what they feel most comfortable with.
Some surgeons tend to use intra operative X-rays to check component positioning and optimal cup seating. The author of this technique had been fellowship trained in DAA and had been involved in over 250 DAA joint replacements before attempting it and was comfortable with cup placement to achieve optimal inclination and anterversion. This was confirmed on the post operative X-rays with no inclination beyond 45 degrees and anteversion beyond 20 degrees on AP and lateral films.
With respect to the scars, all patients were happy with no increased risk of infection despite being adjacent to the groin area.
LIMITATIONS
Initially there was bias in selecting thinner patients for the approach but with time almost all patients underwent the bikini approach.
Functional outcome scores would be very helpful in determining if this soft tissue sparing approach was superior. At the start of the study, the first group of patients did not have the rigorous post-operative scores determined although subsequent patients did and will be the basis of another study.
CONCLUSION
REFERENCES
- Rachbauer F, Kain MS, Leunig M (2009) The history of the anterior approach to the hip. Orthop Clin North Am 40: 311-320.
- Smith-Petersen MN (1917) A new supra-articular subperiosteal approach to the hip joint. Am J Orthop Surg 215: 592-595.
- Judet J, Judet R (1950) The use of an artificial femoral head for arthroplasty of the hip joint. J Bone Joint Surg Br 32: 166-173.
- Bremer AK, Kalberer F, Pfirrmann CW, Dora C (2011) Soft-tissue changes in hip abductor muscles and tendons after total hip replacement: Comparison between the direct anterior and the transgluteal approaches. J Bone Joint Surg Br 93: 886-889.
- Bergin PF, Doppelt JD, Kephart CJ, Benke MT, Graeter JH, et al. (2011) Comparison of minimally invasive direct anterior versus posterior total hip arthroplasty based on inflammation and muscle damage markers. J Bone Joint Surg Am 93: 1392-1398.
- Meneghini RM, Pagnano MW, Trousdale RT, HozackWJ (2006) Muscle damage during MIS total hip arthroplasty: Smith-Petersen versus posterior approach. Clin Orthop Relat Res 453: 293-298.
- Barrett WP, Turner SE, Leopold JP (2013) Prospective randomized study of direct anterior vs postero-lateral approach for total hip arthroplasty. J Arthroplasty 28: 1634-1638.
- Taunton MJ, Mason JB, Odum SM, Springer BD (2014) Direct anterior total hip arthroplasty yields more rapid voluntary cessation of all walking aids: a prospective, randomized clinical trial. J Arthroplasty 29: 169-172.
- Mayr E, Nogler M, Benedetti MG, Kessler O, Reinthaler A, et al. (2009) A prospective randomized assessment of earlier functional recovery in THA patients treated by minimally invasive direct anterior approach: A gait analysis study. Clin Biomech (Bristol, Avon) 24: 812-818.
- Martin CT, Pugely AJ, Gao Y, Clark CR (2013) A comparison of hospital length of stay and short-term morbidity between the anterior and the posterior approaches to total hip arthroplasty. J Arthroplasty 28: 849-854.
- Leunig M, Faas M, von Knoch F, Naal FD (2013) Skin crease ‘bikini’ incision for anterior approach total hip arthroplasty: surgical technique and preliminary results. Clin Orthop Relat Res 471: 2245-2252.
- Spaans AJ, van den Hout JA, Bolder SB (2012) High complication rate in the early experience of minimally invasive total hip arthroplasty by the direct anterior approach. Acta Orthop 83: 342-346.
- Bhargava T, Goytia RN, Jones LC, Hungerford MW (2010) Lateral femoral cutaneous nerve impairment after direct anterior approach for total hip arthroplasty. Orthopedics 33: 472.
- Goulding K, Beaulé PE, Kim PR, Fazekas A (2010) Incidence of lateral femoral cutaneous nerve neurapraxia after anterior approach hip arthroplasty. Clin Orthop Relat Res 468: 2397-2404.
- Kerr D, Kohan L (2008) Local infiltration analgesia: a technique for the control of acute postoperative pain following knee and hip surgery: a case study of 325 patients. Acta Orthop 79: 174-183.
Citation: Nizam I (2015) The Bikini Hip Replacement - Surgical Technique Preserving Vessels and Deep Soft Tissues in Direct Anterior Approach Hip Replacement. J Orthop Res Physiother 2: 007.
Copyright: © 2015 Ikram Nizam, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.

