
A Prospective Randomized Comparative Study between the Self-Pressurized Air-Q with Blocker and Air-Q Blocker in Female Patients Undergoing Minor Gynaecological Procedures
*Corresponding Author(s):
Nesrine Abdel Rahman El-RefaiDepartment Of Anesthesia, Intensive Care And Pain Management, Faculty Of Medicine, Cairo University, Egypt
Tel:+20 1001775623,
Email:nesrinerefai@hotmail.com
Abstract
Background: Supraglottic Airway Devices (SAD) have become valuable for both routine and difficult airway management, Air-q is an intubating laryngeal airway allowing passage of conventional endotracheal tubes (up to 7.5- and 8.5-mm IDs for Air-Q sizes 3.5 and 4.5, respectively).
Methods: This randomized comparative study was conducted in obstetrics and gynecology department, Kasr Al-Ainy hospital, Faculty of Medicine, Cairo University, Egypt. Patients were allocated into 2 equal groups of 30 patients each. Random allocation numbers were concealed in opaque closed envelops. Patients were allocated as follows
• GSPB (n=30): size 3.5 or 4.5 AIR Q SP with blocker was selected and used as a ventilating SGD according to manufacturer’s recommendations.
• GB (n=30): size 3.5 or 4.5 AIR Q blocker was selected and used as a ventilating SGD according to manufacturer’s recommendations. Proper positioning was confirmed by inspection of chest inflation bilaterally, auscultation of the chest bilaterally, auscultation of the neck for abnormal respiratory sounds, absence of any leak sounds from the device and a successive stable square-waves in capnogram trace.
Results: In this study 60 patients were randomly allocated into two equal groups of 30 each. There was no statistically significant difference regarding mean age, mean body weight and El-Ganzouri score between the studied groups. While studying the Airway Seal Pressure (primary outcome) at different time intervals did not show significant difference between the 2 study groups. Furthermore, there was statistically significant decrease in GSPB when compared to GB throughout all time intervals (p < 0.001). In both groups mean blood pressure decreased while mean heart rate increased after induction with no statistical significance between the two groups. Only 3.3% in each group showed postoperative complications in the form of bloody mucus and was not statistically significant.
Conclusion: Air Q MLA with blocker offered a better airway sealing pressure than air Q MLA SP with blocker together with shorted insertion time.
Keywords
Air-Q blocker; Female patients; The self-pressurized Air-Q with blocker
INTRODUCTION
Supraglottic Airway Devices (SAD) has become valuable for both routine and difficult airway management. Air-q is an intubating laryngeal airway allowing passage of conventional endotracheal tubes (up to 7.5- and 8.5-mm IDs for Air-Q sizes 3.5 and 4.5, respectively). The Air-Q family has introduced many improved designs, among which the Air-Q blocker intubating laryngeal airway (Reusable Air-Q Masked Laryngeal Airway with blocker, Daniel j cook, Cook gas, USA) in 2011 [1,2]. They have a soft side channel with a specific upper esophageal blocker tube for accessing the stomach, by suction or venting (Figure 1).
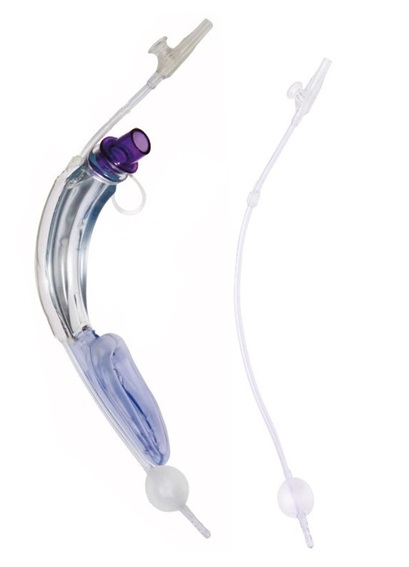
Figure 1: Air Q-blocker.
Air q blocker SP has provided a good seal for ventilation at lower gas flows, with minimal air leak to the esophagus and consequently minimal rise in intragastric pressure thus preventing regurgitation (Figure 2) [3,4]. The new Air-Q blocker SP (Reusable self-pressurized Air-Q Masked Laryngeal Airway with blocker, Daniel j cook, Cook gas, USA.) has the same side-channel but no pilot balloon or inflating cuff. The Air-Q blocker SP incorporates a self-regulating periglottic cuff at the end of this tube, a communication orifice at the junction of the periglottic cuff and the airway tube [5]. This communication between two spaces enables the cuff to dynamically regulate intra-cuff pressure depending on airway pressure. This distinguishing feature of the Air-Q blocker SP may result in reduced risk of airway morbidities related to cuff hyperinflation [6].

Figure 2: Air Q SP blocker.
Hypothesis
It was hypothesized that the Air-QILA blocker SP offers a sealing pressure as high as the Air-QILA blocker in patients undergoing minor gynecological surgeries under general anesthesia with muscle relaxation.
Aim of the study
To compare the new Air-Q MLA blocker SP to the old one Air-Q blocker Mask laryngeal airway (Air-Q MLA blocker) regarding airway sealing pressure 10 minutes after insertion as the primary outcome. Furthermore, Airway Seal Pressure after insertion and after completion of surgery was also recorded for both groups. Insertion variables (ease, time of device insertion and number of attempts of device insertion) together with any associated complications namely blood-streaked mucus, hypoxemia (SpO2 < 90%), gastric insufflations and sore throat were recorded for both groups as secondary outcomes.
METHODS
This randomized comparative study was conducted in the obstetrics and gynecology department, Kasr Al-Ainy Hospital, Faculty of Medicine, Cairo University, Egypt. After obtaining agreement of local department ethics committee and the study was registered with the Clinical Trials.gov ID: NCT03816969) (before patient enrolment), and obtaining an informed written consent from the patients, 60 female patients between ages 18 to 50 years, ASA I and ASA II, with El-Ganzouri score < 3, undergoing elective ambulatory surgeries in obstetrics and gynecology theatre in the lithotomy position at Kasr Al-Ainy hospital were enrolled in the study [7]. However, patients with ASA III - V patients, Airway score ≥ 3 according to Ganzouri Airway Scoring System, patients with any or pharyngeal pathology, patients known to have a risk of gastric aspiration, gastroesophageal reflux disease, hiatus hernia or previous upper gastrointestinal tract surgery were excluded from the study [7]. An online randomization program (http://www.randomizer.org) was used to generate random lists and patients were allocated into 2 equal groups of 30 patients each. Random allocation numbers were concealed in opaque closed envelopes. The patient and investigator assessing study outcomes were all blinded to the study groups’ allocation. Patients were allocated as follows
• GSPB (n=30): size 3.5 or 4.5 AIR Q SP with blocker was selected and used as a ventilating SGD according to manufacturer’s recommendations
• GB (n=30): size 3.5 or 4.5 AIR Q blocker was selected and used as a ventilating SGD according to the manufacturer’s recommendations.
• The device was adequately lubricated with K- y gel.
In the preoperative preparation room, proper airway assessment of all patients was done according to El-Ganzouri Airway Scoring System ( 7) to exclude patients with suspected difficult intubation. An IV cannula was inserted in a peripheral vein and all included patients received metoclopramide 10mg IV 1 hour before the operation, intravenous atropine 0.01mg/Kg 20 minutes before induction and IV midazolam 0.02mg/Kg just before induction.
In the operating room, basic monitoring was established namely pulse oximeter, electrocardiogram, non-invasive blood pressure, and peripheral nerve stimulator. After 3 minutes of adequate preoxygenation with 100% mask oxygen, anesthesia was induced by Lidocaine 1mg/kg, Fentanyl 2Ug/kg, Propofol 2mg/kg, and atracurium 0.5mg/kg. Mechanical ventilation was maintained with a Tidal volume of 6 ml/kg and a rate of 12 / min with isoflurane 1.5% Mac and 100% oxygen for at least 3 additional minutes by a face mask. After complete muscle relaxation (TOFC=0), and according to the patient’s group, the selected proper sized supraglottic device was inserted in the patient's oropharynx and connected to capnography. Proper size selection and insertion techniques were based on the manufacturer's recommendations.
Device insertion was considered successful by observing bilateral chest wall movement, bilateral equal air entry by stethoscope as well as a successive stable square-wave in capnogram trace. Proper insertion was also confirmed by the absence of adventitious sounds over the neck as a sign of air leak or decrease in SPO2 < 92%.
If improper insertion had been encountered, external manipulation of the device was tried before its removal in the form of side to side movement or slightly pulling out or pushing down the device to improve its position. If external manipulation failed, the device was removed, and a new insertion attempt was performed after adequate ventilation of the patient to increase the SPO2 > 98%. Only 2 attempts were allowed for device insertion, otherwise, the case was considered as a failed trial and the patient was withdrawn from the study. The device insertion time was recorded (defined as the time elapsing from opening the patient’s mouth until the removal of the assessor’s hand after device insertion into the oropharynx).
The ease of device insertion was recorded and graded on a scale of 1-3 (1 = easy, 2 = moderate, 3 = difficult). (1) Easy means obtaining an effective airway (defined as normal chest movement and a square wave capnograph trace) from the first attempt. (2) Moderate means obtaining an effective airway in the first attempt with external manipulation of the device after insertion to ensure proper sealing. (3) Difficult means obtaining an effective airway in the second attempt with or without external manipulation of the device after insertion [8]. The Airway Seal Pressure (ASP), which describes the seal pressure above which air leak occurs and a sound can be heard from around the SGD while auscultating the anterior of the neck or a release sound can be heard near the mouth opening [9].
The seal pressure test
While the patient’s head in the neutral position, the airway seal pressure was tested by closing the adjustable pressure-limiting expiratory valve to 70 cm H2O of the circle system, with fresh gas flow rate adjusted at 3L/min, while observing the gradually rising pressure gauge of the calibrated manometer in the expiratory limb of the anesthesia machine circle system, until a sudden release of pressure with an audible puffing sound was heard near the angle of mouth [10]. This pressure was recorded as the pressure at which the leak occurred. The seal pressure of the device will be less by (1 cm H2O) [10]. Proper positioning was confirmed by inspection of chest inflation bilaterally, auscultation of the chest bilaterally, auscultation of the neck for abnormal respiratory sounds, absence of any leak sounds from the device and a successive stable square-waves in capnogram trace.
During anesthesia complications including hypoxemia (Saturation < 90%), airway obstruction due to improper positioning, gastric insufflations (recorded by the presence of air sounds during epigastric auscultation with lung inflation) were recorded. Any postoperative complications such as sore throat, dysphagia, and blood-streaked mucus over the device after its removal were also recorded in both groups. A blinded investigator-assessed all patients in the post-anesthesia care unit PACU.
Primary outcome: The Airway Seal Pressure (ASP) after insertion.
Secondary outcome(s):
• Airway Seal Pressure after completion of surgery.
• Insertion variables (ease, time of device insertion and number of attempts of device insertion).
• Complications associated (blood-streaked mucus, hypoxemia (SpO2 < 90%), gastric insufflation, and sore throat)
Sample size
Depending on a previous study, the mean (SD) of sealing pressure with air Q blocker was 22.4 ± 1.27 cm H2O. We assumed a difference of 10% with other groups. G power software (version 3.1.3, Germany) was used with alpha error 0.05 and power of 95% and doubling of SD, the sample size will be 26 per group to be increased to be 30 per group for possible dropouts [11].
Statistical analysis
Categorical data were described as numbers (frequency) and were analyzed by the chi-square test. Continuous data were described as mean (standard deviation) and were analyzed by T testing. For all statistical comparisons, a p-value less than or equal to 0.05 was considered to be significant. Data entered by qualified research assistants and data entry. All data analysis and graphical demonstrations were done, using the statistical package for social sciences SPSS version 24 software.
RESULTS
Of 63 enrolled patients, 60 patients were included in the study. The flow chart of the patients through the study followed the CONSORT flow diagram is presented in figure 3. Demographic characteristics for age, ASA and Anthropometric measures were presented in table 1. In this study 60 patients were randomly allocated into two equal groups of 30 each:
• GSPB (n=30): size 3.5 or 4.5 AIR Q SP with blocker was selected and used as a ventilating SGD according to manufacturer’s recommendations.
• The GB (n=30): size 3.5 or 4.5 AIR Q SP blocker was selected and used as a ventilating SGD according to the manufacturer’s recommendatiions.
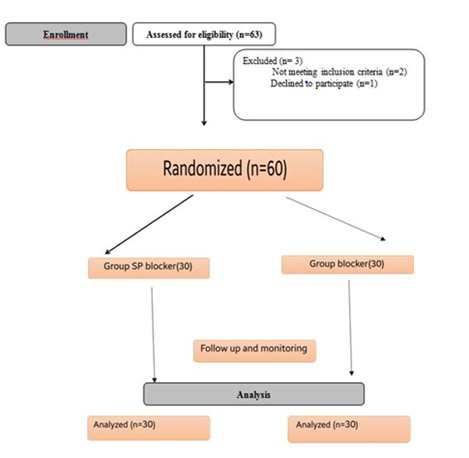
Figure 3: Consort Flow Diagram.
There were no statistically significant differences regarding mean age, mean body weight, and El-Ganzouri score between the studied groups (Table 1,2).
|
Group |
Group SP Blocker |
Group Blocker |
P value |
|||
|
Variables |
No |
% |
No |
% |
||
|
Age (yrs) |
Mean ± SD |
27.6 ± 7.3 |
31.7 ± 8.6 |
0.051 |
||
|
Weight (kg) |
Mean ± SD |
72.0 ± 8.2 |
69.7 ± 8.5 |
0.296 |
||
|
Range |
60 - 90 |
55 - 85 |
|
|||
Table 1: Descriptive statistics for the demographic data of the tested groups.
Numerical data are presented as mean ± SD p < 0.05 was considered statistically significant.
|
|
SP Blocker |
Blocker |
P value |
||||
|
Median |
Min |
Max |
Median |
Min |
Max |
|
|
|
Ganzouri score |
1 |
1 |
2 |
2 |
1 |
2 |
0.798 |
Table 2: El-Ganzouri score.
While studying the Airway Seal Pressure (primary outcome) at different time intervals for each device, it remained constant at different time intervals. Furthermore, there was a statistically significant decrease in GSPB when compared to GB throughout all time intervals (p < 0.001). (Figure 4, Table 3).
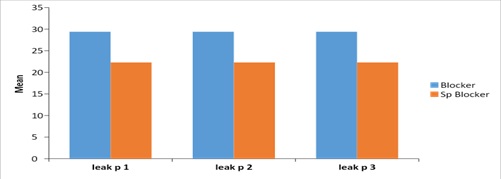
Figure 4: Significant difference in Airway seal pressure between 2 groups.
|
|
GSpB |
GB |
|
|
Mean ± SD |
Mean ± SD |
p value |
|
|
ASP1 at insertion |
22.3 ± 3.3 |
29.4 ± 4.7 |
< 0.001* |
|
ASP 2 after 10 min |
22.3 ± 3.3 |
29.4 ± 4.7 |
< 0.001* |
|
ASP 3 at the end of surgery |
22.3 ± 3.3 |
29.4 ± 4.7 |
< 0.001* |
Table 3: Airway Seal Pressure (ASP) readings in the studied groups.
Numerical data are presented as mean ± SD. p < 0.05 was considered statistically significant.
*Denotes statistically significant.
Time of insertion and number of attempts:
Only 3.3% in each group showed postoperative complications in the form of bloody mucus and was not statistically significant (Table 4).
|
Group |
GSpB |
GB |
P value |
|||
|
Variables |
||||||
|
Time (sec) |
Mean ± SD |
9.2 ± 2.1 |
8.4 ± 1.6 |
0.098 |
||
|
|
No |
% |
No |
% |
|
|
|
Number of Trials |
1 |
29 |
96.7 |
29 |
96.7 |
1 |
|
2 |
1 |
3.3 |
1 |
3.3 |
||
Table 4: Comparison between time of insertion, number of trials and ease of insertion in studied groups.
In both groups mean blood pressure decreased while the mean heart rate increased after induction with no statistical significance between the two groups (Table 5,6).
|
|
GSpB |
GB |
|
|
|
|
Mean ± SD |
Mean ± SD |
P value |
|
|
MAP base |
79.6 ± 2.3 |
80.3 ± 1.7 |
0.163 |
|
|
MAP induction |
74.4 ± 2.9 |
73.7 ± 3.0 |
0.36 |
|
|
MAP insertion |
73.0 ± 4.5 |
71.3 ± 4.5 |
0.148 |
|
|
MAP removal |
76.0 ± 4.5 |
75.3 ± 5.4 |
0.439 |
Table 5: Mean arterial pressure (MAP) readings in studied groups.
Numerical data were presented as mean ± SD. p < 0.05 was considered statistically significant.
|
|
GSPB |
GB |
|
|
|
Mean ± SD |
Mean ± SD |
P value |
|
HR base |
84.8 ± 4.7 |
86.1 ± 5.4 |
0.337 |
|
HR induction |
90.4 ± 6.4 |
91.6 ± 7.1 |
0.494 |
|
HR insertion |
87.6 ± 6.5 |
90.8 ± 5.9 |
0.061 |
|
HR removal |
90.9 ± 7.1 |
93.7 ± 5.9 |
0.096 |
Table 6: Heart Rate (HR) readings in studied groups.
Numerical data are presented as mean ± SD. p < 0.05 was considered statistically significant.
Only 3.3% in each group showed postoperative complications in the form of bloody mucus and was not statistically significant (Table 7).
|
|
GSPB |
GB |
P value |
|||
|
No |
% |
No |
% |
|||
|
Number of patients |
1(bloody mucus) |
3.3 |
1(bloody mucus) |
3.3 |
1 |
|
Table 7: Incidence of postoperative complications in studied groups.
DISCUSSION
In this study we reported that air Q MLA with Blocker (GB) provided a better sealing pressure than air Q MLA SP with Blocker (GSPB). Furthermore, there were no significant differences between both devices in the mean time of device insertion, number of insertion attempts, ease of insertion and complications. To the best of our knowledge, this is the first study to compare the air Q MLA blocker to the air Q MLA SP blocker. Regarding Airway Seal Pressure, in the current study, we found that the seal pressure in GB was favorably higher than GSPB (29.4 ± 4.7 cmH20 vs. 22.3 ± 3.3cmH2O respectively). This was statistically significant (P < 0.001). Similar to our results, Galgon RE, et al, who compared air Q MLA classic, and air Q MLA classic SP, found that the seal pressure recorded was 28 ± 6 and 27 ± 8 cmH2O respectively [2]. However, the study did not use the blocker version of the air Q MLA, also 60.9% of the participants of this study were males (n=137) compared to our study in which all participants (n=60) were females. Similar to Galgon et al, they found that the airway seal pressures for the Air-Q classic were 30 ± 7 cmH2O in a comparative study between air Q classic and LMA proseal [11]. Furthermore, Srinath Damodaran et al, showed that the seal pressure of air q device was 26 ± 5 cmH2O in Comparative study between air-Q™, I-gel™, and laryngeal mask airway.
In contrast to our study, Youssef MMI, et al. compared LMA-Proseal™ and Air-Q® Blocker for ventilation in adult eye trauma patients, found that the seal pressure of the air Q MLA with blocker was 22.4 ± 1.27 cm H2O [13]. This might be attributed to anatomical differences of the larynx in both genders; more than 50% of their cases were male’s vs. 100% females in our study. Also, Jagannathan et al, who compared air Q MLA SP to LMA unique in children, showed that the air Q SP leak pressure was 16 ± 2 cm H2O at the time of insertion [4]. This difference in pressure may be related to the use of Air Q MLA classic version and the different age groups in their study being performed on children (3-9 years) vs. adult females (18-50 years) in the current study. Concerning mean time for device insertion, in the current study, the time was 9.2 ± 2.1 sec in GSPB and 8.4 ± 1.6 sec in GB.
This was in accordance with Jagannathan et al, who found that time for insertion of air Q was 12 ± 2 sec [5]. On the contrary, Youssef MMI et al, found that the insertion time of air q with blocker was 18.37 ± 3.77 sec [13]. This difference in insertion time can be explained by the differences in calculating the time of insertion, their time of insertion had been starting from the removal of mask ventilation until the appearance of the first capnography wave. However, in our study the time was calculated from opening the patient’s mouth to removal of the assessor’s hand after device insertion into the pharynx and this time was surely shorter. With the reference to number of attempts of device insertion, in the current study, in GB, the device was inserted from the first attempt in 96.7% of the cases. These results coincide with the results by Youssef MMI, et al, where the air Q blocker was inserted easily from the first attempt in 90% of cases [13].
Similar results were recorded by Jagannathan et al, who showed a first trial success rate of 100% in air Q SP [5]. As for complications in this study, only 2 cases, one patient (3.3%) in each group was found to have postoperative blood-streaked mucus over the device. No other complications were reported. In accordance with our study results, El-Ganzouri et al, found in his study that 3.3% had blood-stained mucus in the air Q group, also Jagannathan et al, reported zero complications while using air Q SP [5,15]. On contrary to the study results, Bakker et al, revealed that 10% of patients of air Q classic group were noted to have dysphagia and one patient was diagnosed with bilateral lingual nerve injury but made a complete recovery in four weeks [16]. Consequently, Joffe et al, study showed that 26% of patients complained of mild sore throat postoperatively before discharge [17].
Our study had some limitations, first the patients’ gender (only females were included in the study) , second, the patients’ position due to the type of surgery (gynecological surgeries) that required a lithotomy position most of the time which might have affected our results. We recommend the reputation of this study on both genders due to differences in the anatomical size of the larynx between the male and female and in patients in different positions not only lithotomy position.
CONCLUSION
Air Q MLA with blocker offered a better airway sealing pressure than air Q MLA SP with blocker together with shorted insertion time.
CONFLICT OF INTERESTS
None.
ACKNOWLEDGMENTS
Approval was obtained from local research committee of anesthesia, Cairo University and the study was registered with the Clinical Trials.gov ID: NCT03816969).
All authors reviewed and approved the final manuscript.
We thank Dr. Daniel Cook for providing the free samples of the Air Q SP-blocker. We also thank the all personnel of the obstetrics and gynecology theatre, Cairo University for their great help and cooperation.
REFERENCES
- Hernandez MR, Klock PA Jr, Ovassapian A (2012) Evolution of the extraglottic airway: A review of its history, applications, and practical tips for success. Anesth Analg 114: 349-368.
- Galgon RE, Schroeder KM, Han S, Andrei A, Joffe AM (2011) The air-Q® intubating laryngeal airway versus the LMA-ProSeal™: a prospective, randomized trial of airway seal pressure. Anaesthesia 66: 1093-1100.
- Marjot R (1993) Pressure exerted by the laryngeal mask airway cuff upon the pharyngeal mucosa. Br J Anaesth 70: 25-29.
- Jagannathan N, Sohn LE, Mankoo R, Langen KE, Roth AG, et al. (2011) Prospective evaluation of the self-pressurized air-Q intubating laryngeal airway in children. Pediatr Anesth 21: 673-680.
- Jagannathan N, Sohn LE, Sawardekar A, Shah R, Ryan K, et al. (2012) A randomised comparison of the self-pressurised air-QTM intubating laryngeal airway with the LMA Unique in children. Anaesthesia 67: 973-979.
- Rieger A, Brunne B, Striebel HW (1997) Intracuff pressures do not predict laryngopharyngeal discomfort after use of the laryngeal mask airway. Anesthesiology 87: 63-67.
- Corso RM, Cattano D, Buccioli M, Carretta E, Maitan S (2016) Post analysis simulated correlation of the El-Ganzouri airway difficulty score with difficult airway. Braz J Anesthesiol 66: 298-303.
- Abdel-Halim TM, Abo El Enin MA, Elgoushi MM, Afifi MG, Atwa HS (2014) Comparative study between Air-Q and Intubating Laryngeal Mask Airway when used as conduit for fiber-optic. Egyptian Journal of Anaesthesia 30: 107-113.
- Mittal RK (2012) Motor Function of the Pharynx, the Esophagus, and Its Sphincters. In: Physiology of the Gastrointestinal Tract.
- Nishimura T, Suzuki K (2003) Anatomy of oral respiration: morphology of the oral cavity and pharynx. Acta Otolaryngol Suppl 550: 25-28.
- Galgon RE, Schroeder K, Joffe AM (2012) The self-pressurising air-Q(R) Intubating Laryngeal Airway for airway maintenance during anaesthesia in adults: a report of the first 100 uses. Anaesth Intensive Care 40: 1023-1027.
- Damodaran S, Sethi S, Malhotra S, Samra T, Maitra S, et al. (2017) Comparison of oropharyngeal leak pressure of air-QTM, I-gelTM, and laryngeal mask airway supremeTM in adult patients during general anesthesia: A randomized controlled trial. Saudi J Anaesth 11: 390-395.
- Youssef MMI, Lofty M, Hammad Y, Elmenshawy E (2014) Comparative study between LMA-Proseal™ and Air-Q® Blocker for ventilation in adult eye trauma patients. Egypt J Anaesth 30: 227-233.
- Hagberg CA (2002) Special devices and techniques. Anesthesiol Clin of North Am 20: 907-932.
- Elganzouri AR, Marzouk S, Youssef MMI, Abdelalem N (2012) The use of AIR-Q as conduit for fiberoptic endotracheal intubation in adult paralyzed patients. Egypt J Anaesth 28: 249-255.
- Bakker EJ, Valkenburg M, Galvin EM (2010) Pilot study of the air-Q intubating laryngeal airway in clinical use. Anaesth Intensive Care 38: 346-348.
- Joffe AM, Liew EC, Galgon RE, Viernes D, Treggiari MM (2011) The second-generation air-Q intubating laryngeal mask for airway maintenance during anaesthesia in adults: a report of the first 70 uses. Anaesth Intensive Care 39: 40-45.
Citation: Shehata JI, El-Refai NA, MI Yousef, Dobal NA, Mohamed AA, et al. (2020) A Prospective Randomized Comparative Study between the Self-Pressurized Air-Q with Blocker and Air-Q Blocker in Female Patients Undergoing Minor Gynaecological Procedures. J Anesth Clin Care 7: 047.
Copyright: © 2020 Shehata JI, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.

