
Management of the Homicidal Cut Throat: An Open Airway Injury
*Corresponding Author(s):
Moktan Sushila LamaLecturer, Kathmandu Medical College And Teaching Hospital, Kathmandu, Nepal
Tel:+977-9841466499,
Email:sushidagreat@hotmail.com
INTRODUCTION
Homicidal cut-throat injuries by definition are injuries over the front of neck by sharp instruments using a long blade with a murderous intent. Neck being relatively unprotected anatomic region is a common site for injuries that are potentially dangerous and require immediate management. Patients may present with acute blood loss due to injury to major vessels, airway compromise, and aspiration. Early intervention could save patient’s life in majority of cases. Management of cut throat injuries requires a multidisciplinary approach. The role of an anesthesiologist is to establish an airway by endotracheal intubation or tracheostomy before wound exploration and repair of transected tissues.
CASE REPORT
An 18-year-old male patient came to the emergency room with the homicidal cut-throat to his anterior neck. The injury had occurred about two hours ago and was referred from another hospital with the loose dressing insitu over the wound which was soaked with blood and the secretions. In the emergency room, patient was agitated and restless but not in respiratory distress and was unable to lie in supine position. The wound was horizontal just above the level of vocal cords over the infrahyoid region exposing the vocal cords. Major blood vessels in the neck were spared and esophagus was found not injured. There was no crepitus, stridor or subcutaneous emphysema, and the neurological examination was normal. There was no other apparent injury to the body. His Blood pressure was 110/60 mm Hg, pulse rate 102/min; oxygen saturation was 94% without oxygen, and respiratory rate 26/min (Figure 1).
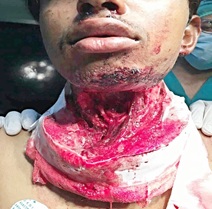 Figure 1: Original picture of patient with homicidal cut-throat.
Figure 1: Original picture of patient with homicidal cut-throat.
The patient was immediately shifted to the operating room after the laboratory investigations and the arrangement of blood products. In the operation theatre, the patient was monitored with multi parameter monitoring like ECG, Pulse oximeter, non-invasive blood pressure and two wide bore intravenous cannula were opened. Injection ranitidine 50mg, injection metoclopramide 10 mg and, injection dexamethasone 6mg was given. Since there were increased chances of foreign body or blood clot in the airway distal to the injury, a thorough and gentle suctioning was done. Once checked the patency of the airway, a 7.5mm internal diameter flexometallic tube was placed through the opening end of the larynx after sedating patient with 2mg of midazolam, 30mg ketamine and 30mg Propofol, with patient supported in sitting position as the patient was unable to lie supine due to injury. Patient was breathing spontaneously and was able to ventilate (Figure 2).
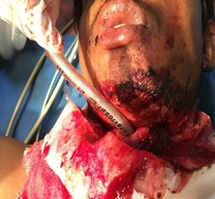 Figure 2: Patient intubated through the open end of the wound.
Figure 2: Patient intubated through the open end of the wound.
Then after the patient was placed in supine position, injection Propofol 50mg, injection Fentanyl 100mcg and isoflurane was given. In the deeper plane, laryngoscopy and orotracheal intubation was done with the removal of the first tube for the proper surgical field. Anesthesia was maintained with vecuronium, isoflurane with IPPV throughout the procedure (Figure 3).
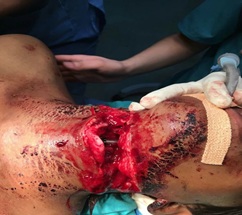 Figure 3: Orotracheal intubation after removal of the first endotracheal tube.
Figure 3: Orotracheal intubation after removal of the first endotracheal tube.
Examination of wound under anesthesia revealed a severe disruption of anterior larynx with fracture in the thyroid and cricoid cartilage along with severe mucosal disruption but the major vessels were intact. The patient was transferred to intensive care unit intubated, and was weaned subsequently without complication. Patient was able to talk with the partial closure of the tracheostomy tube, so, gradually tracheal decannulation was done (Figures 4 and 5).
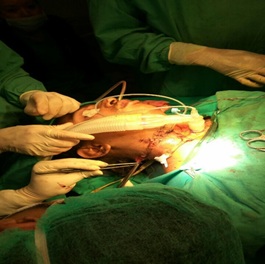 Figure 4: Repaired wound with tracheostomy.
Figure 4: Repaired wound with tracheostomy.
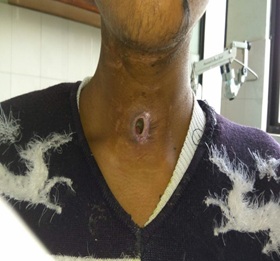 Figure 5: Tracheal decannulation.
Figure 5: Tracheal decannulation.
DISCUSSION
Homicidal cut-throat injuries are usually inflicted by the sharp items and the wound may be open or incised or simulate as incised injuries. Homicidal cut throat injuries are not uncommon, but literature about its incidence and survival rate is not available. Major neck vessels and the vital structures that course through this area make these injuries potentially life threatening. Such injuries mainly have airway compromise and injury to the vasculature [1,2]. Therefore clinical examination and investigations should be aimed to detect injury to these structures. The investigations should include, X-ray of the neck and chest, computed tomography scan, bronchoscopy and barium swallow. But these radiological studies should not delay the airway management as an apparently stable airway can rapidly progress into an acute airway obstruction [3,4].
Though our patient was apparently stable and breathing spontaneously, sometimes they may rapidly deteriorate due to fatal airway distortion because of subcutaneous emphysemas, hematomas and soft tissue swelling. So, the patient was immediately taken to operation theatre. On examining the neck, a horizontal cut-throat wound of around 14 cm×4 cm size, extending from the posterior border of the sternocleidomastoid muscle to the opposite side sternocleidomastoid muscle, was seen. Thyroid and cricoid cartilage was fractured and vocal cords were exposed noted along with the severe disruption of mucosa but there was no active bleed. As there is increased chance of foreign body like blood clot, chipped cartilages and also the thick secretions, we meticulously suctioned through the exposed open vocal cord. Our backup plan was to do fibreoptic bronchoscopy if we had encountered any resistance during suctioning. We considered intubating the patient through the vocal cords exposed outside through the cut-throat injury with cuffed endotracheal tube under sedation with patient supported from behind in sitting position as he was unable to lie supine. Awake oral intubation utilizing topical analgesia and fiber optic bronchoscope have in such cases been advocated [5,6]. Later, after keeping the patient in supine position, patient was given an injection Propofol, injection fentanyl, and isoflurane, then another flexometallic endotracheal tube was passed through the oral route then exchanged with the initial tube for proper surgical exposure. Exploration of the neck wound was done by an experienced otolaryngologist under general anesthesia. Nasogastric tube was inserted, stoma was made in the trachea and the wound was closed in layers.
The patient was shifted to the ICU and mechanical ventilation was continued for about 10 hours post-operatively after which he was weaned off the ventilator. The tracheostomy tube was removed and the patient was decannulated after two weeks. With a good quality of voice and ability to swallow, the patients were discharged home three weeks after the admission.
CONCLUSION
Airway trauma is rare but life threatening injury. The first priority is to establish and maintain stable airway. Early decision and intervention to secure the airway, not only permits a controlled milieu for resuscitation but is also prudent to avoid any catastrophic airway compromise. Immediate care and adequate surgical repair are vital for treating such life threatening injuries.
REFERENCES
- Herzog M, Hoppe F, Baier G, Dieler R (2005) Injuries of the head and neck in suicidal intention. Laryngorhinootologie 84: 176-181.
- Bhargava AK, Gandhi BK, Mahajan HK (1998) Anaesthetic management in cut throat injuries (A report of two cases). Med J Armed Forces India 54: 53-54.
- Rao PM, Noveline RA, Doblins JM (1966) The spherical endotracheal tube cuff: A plain radiographic sign of tracheal injury. Emergency Radiology 3: 87-90.
- Gonzalez RP, Falimirski M, Holevar MR, Turk B (2003) Penetrating zone II neck injury: does dynamic computed tomographic scan contribute to the diagnostic sensitivity of physical examination for surgically significant injury? A prospective blinded study. J Trauma 54: 61-65.
- Chitragupta AP (2016) Management of Homicidal Cut Throat Injury at a Peripheral Set up: A Case Report. J Perioper Crit Intensive Care Nurs 2: 133.
- Peralta R, Hurford WE (2000) Airway trauma. IntAnesthesiol Clin 38: 111-127.
Citation: Lama MS (2019) Management of the Homicidal Cut Throat: An Open Airway Injury. J Anesth Clin Care 6: 42.
Copyright: © 2019 Moktan Sushila Lama, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.

