
Clinical Image - Unexplained Intraluminal Contrast in a Trauma Patient
*Corresponding Author(s):
Lauren RaffDepartment Of General Surgery, Health Care Hernia Center, The University Of North Carolina, Chapel Hill, NC, United States
Tel:919-966-4389,
Fax:919-966-0389
Email:lauren_raff@med.unc.edu
CLINICAL IMAGE
A 22-year-old male presented from the scene as a trauma after motorcycle crash. He was tachycardic and hypertensive with obvious extremity injuries and a circular handlebar injury to the midabdomen. He underwent CT scan with intravenous contrast. CT revealed free intraperitoneal air with intraluminal high-density material consistent with contrast in the small and large bowel. However, the patient did not receive oral contrast, nor had he had any recent imaging. He was taken to the operating room and underwent exploratory laparotomy. A jejunal perforation was identified and resected, but did not completely explain the intraluminal contrast. Only after exploring the remaining GI tract, mobilizing the right colon, and performing a Kocher maneuver, was it possible to identify the etiology of the intraluminal contrast. There was a 3 centimeter duodenal perforation with an adjacent actively bleeding branch off of the superior mesenteric vein. The venous branch was suture ligated and the duodenal perforation closed in two layers. The patient was left in discontinuity with an open abdomen, secondary to intraoperative pressor requirements, and was taken the following day to the operating room for reanastomosis and a second look. During that procedure, the duodenal anastomosis was evaluated and appeared healthy and intact. There was no evidence of ongoing bleeding from the previously ligated mesenteric vein branch. No further venography was performed.
Due to timing of the CT imaging, there was no evidence of extravasation of IV contrast from the venous injury into the duodenal perforation, but there was clear evidence of contrast in the GI tract in the absence of PO contrast administration. The injury pattern is somewhat unique in that the venous bleeding was entirely into the GI tract rather than intraabdominal. However, given the trajectory of the high impact blunt injury from the motorcycle handlebar, the venous branch injury overlying the duodenal branch injury is easily explained. The decision for operative intervention was based on free air and unexplained intraluminal contrast in the GI tract. Although the jejunal perforation explained the free air, further exploration was necessary for discovering the etiology of the intraluminal contrast. This is a useful case presentation on the importance of performing a thorough exploration of the entire GI tract for all trauma patients.
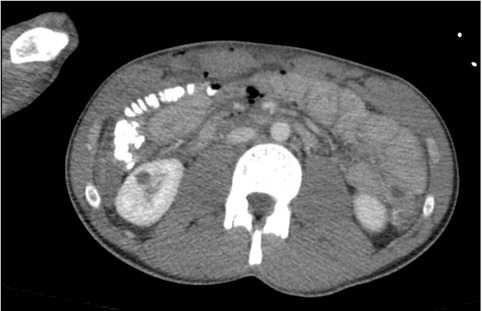
Figure 1: Intraluminal contrast is noted within the cecum and right colon.
There is a small amount of intraabdominal free air and subcutaneous emphysema of the anterior abdominal wall
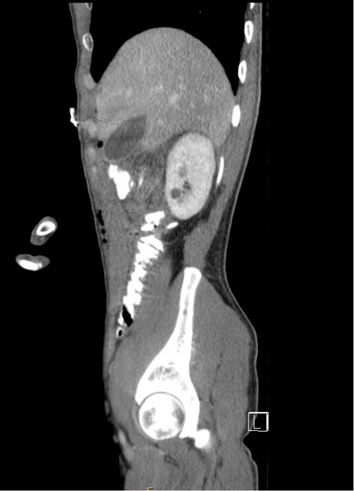
Figure 2: Intraluminal contrast is noted within the right and transverse colon.
There is a small amount of intraabdominal free air and subcutaneous emphysema of the anterior abdominal wall.
Copyright: © 2020 Lauren Raff, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.

