
Past, Present and Future of Tea (Total Elbow Arthroplasty)
*Corresponding Author(s):
Bernardino SaccomanniDepartment Of Orthopedic Clinic, Institution Of Ambulatorio Di Ortopedia, Via Della Conciliazione, 65 Cap 74014 Laterza (Ta), Italy
Tel:+39 3208007854,
Email:bernasacco@yahoo.it
Abstract
In my opinion, the negative bias toward this procedure is no longer warranted. From a clinical standpoint, the majority of patients have marked improvement in function and significant pain relief. TEA has come a long way in the past two decades. Implant survival data nearly approach those of knee arthroplasty. However, the complication rate, higher than for total hip and knee arthroplasty, is likely inherent in the anatomic uniqueness of the elbow itself. With less bone stock for implantation as well as a less robust soft tissue envelope than the hip and knee, the surgeon and patient must exercise greater caution with TEA implantation.
Introduction
The elbow has the most complex articular anatomy of any human joint and is also biomechanically more critical to upper extremity function than the wrist or shoulder. Even minor trauma or transient disease involvement can result in prolonged, limited, if not permanent, painful motion. Although the elbow is not commonly considered a weight-bearing joint, static loading forces can equal 3 times body weight, and dynamic loading can equal 6 times body weight.
The elbow is frequently involved in many diseases, most notably, rheumatoid arthritis. In fact, 20% to 60% of patients with rheumatoid arthritis have elbow involvement. The elbow is also affected by other inflammatory arthropathies, primary degenerative osteoarthritis, crystalline arthropathy, hemophilia, and sepsis. The elbow is frequently injured in both adults and children. Fractures about the elbow account for 7% of all adult fractures, and after the shoulder, the elbow is the second most frequently dislocated joint [1-3]. Historically, some of the earliest surgical procedures to alleviate pain and preserve motion included resection arthroplasty and interposition arthroplasty. Not surprisingly, resection arthroplasty (performed primarily for sepsis) yielded unpredictable functional results. Interposition arthroplasty has been in use since the 1900s. Various autologous tissues (eg, fat, muscle, tendon, fascia) and later nonautologous materials (eg, silicone sheeting, gelatin sponges, xenograft pig bladders) have been used with varying success [4-8]. Today, autogenous cutis interposition grafts continue to be used in younger patients.
Prosthetic Replacement Arthroplasty
Historical Perspective
Even today there exists a negative bias toward total elbow arthroplasty (TEA). A degree of pessimism is warranted, owing to the poor surgical outcomes of early prosthetic designs.
From the late 1940s through the late 1960s, before the use of methacrylate bone cement and polyethylene bearing surfaces, numerous custom-made fully constrained (flexion-extension motion only) hinged implants were developed that relied on both extracortical and intramedullary implant seating [Figure 1]. These implants failed with regularity, secondary to loosening, metallic wear debris, and metal failure [5,6,8-12]. Recognition that the constrained hinge designs were failing at an unacceptable rate led surgeons to develop surface replacement hemiarthroplasty implants for the distal end of the humerus and the proximal ulna [4,13]. Clinical experience with these hemiarthroplasty implants was limited, and few long-term studies were reported.
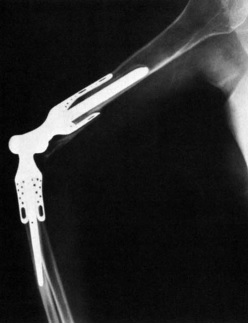 Figure 1: Fully constrained, custom-hinged total elbow arthroplasty with radiographic evidence of loosening (From London JT. Custom arthroplasty and hemiarthroplasty of the elbow. In: Morrey BF, editor. The elbow and its disorders. 2nd ed. Philadelphia: WB Saunders; 1993.)
Figure 1: Fully constrained, custom-hinged total elbow arthroplasty with radiographic evidence of loosening (From London JT. Custom arthroplasty and hemiarthroplasty of the elbow. In: Morrey BF, editor. The elbow and its disorders. 2nd ed. Philadelphia: WB Saunders; 1993.)
The Modern Era
The modern era of TEA, which began in the late 1970s, was heralded by several important developments. The expanded use of high-density polyethylene as a bearing surface to metal and the use of methylmethacrylate bone cement were implemented in TEA following the success of total hip and knee arthroplasty [4,12,14-18]. Equally important was the implementation of sound biomechanical investigations which led to improved designs that attempted to replicate normal joint kinematics, thereby reducing the potential for material wear and implant loosening [8,19].Modern TEA implants fall into two design categories, linked and unlinked. These terms are generally interchangeable with the descriptors semiconstrained and unconstrained, respectively [3,20].Linked implants are coupled together with pins or snap-fit bushings that produce a semiconstrained hinged construction, allowing for a degree of laxity in the medial, lateral, and rotational planes that closely simulates the loose hinge of normal elbow kinematics [5,8,17,21-25] [Figure 2]. Unlinked or unconstrained implants are not mechanically linked but rely on matching shapes of the bearing surfaces, adequate bone stock, and, most importantly, the integrity of present or reconstructable capsular and ligamentous structures [4,15,20,23,26-29] [Figure 3].
 Figure 2: Coonrad-Morrey (Mayo) total elbow arthroplasty prosthesis.
Figure 2: Coonrad-Morrey (Mayo) total elbow arthroplasty prosthesis.
 Figure 3: Capitellocondylar (unconstrained) ulnar component.
Figure 3: Capitellocondylar (unconstrained) ulnar component.
Both linked and unlinked TEA implants have similar indications, including rheumatoid arthritis, posttraumatic arthritis, and degenerative osteoarthritis. Furthermore, both have yielded similar functional outcome and patient satisfaction scores [3,11,12,18,27]. However, because of the inherent differences in stability, the linked and unlinked designs have different indications. The unlinked designs require competent soft tissue constraints and adequate bone stock length to yield a stable arthroplasty. Therefore, their use is often limited to or preferred when there is less bone or articular destruction [Figure 4].
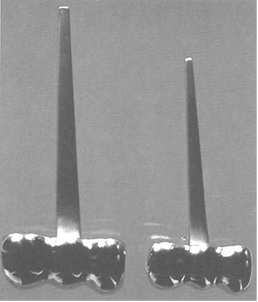 Figure 4: Capitellocondylar (unconstrained) humeral component.
Figure 4: Capitellocondylar (unconstrained) humeral component.
Moreover, as less bone is removed to implant the resurfacing unlinked prosthesis, it may be preferred in younger patients who may need later revision surgery [3,11,15,21].The increased stability of the linked implant designs expands the indications for their use. Specifically, they are now indicated in later stages of rheumatoid arthritis, posttraumatic arthritis, and osteoarthritis where increased bone destruction and ligamentous incompetency exist [2,3,20,25]. Furthermore, the linked implants have broadened indications for distal humerus malunions and nonunions. Additionally, linked implants are indicated for complex displaced intra-articular fractures that are not satisfactorily reassembled by fracture internal fixation techniques, particularly in elderly patients with osteoporotic bone [2].
Contraindications
Absolute contraindications for TEA include flaccid paralysis of the upper extremity and nonrestorable function of the biceps and triceps. Poor patient compliance with activity and weight-lifting restrictions is also an absolute contraindication for surgery. Arthrodesis of the elbow remains a relative contraindication for TEA. Historically, a previous open infected elbow wound or a previously infected TEA were absolute contraindications [23]. However, Yamaguchi et al38 reported that salvage of infected TEA with reimplantation can yield acceptable outcomes in selected patients with specific pathogens.
Surgical Techniques and Postoperative Rehabilitation
The majority of patients who undergo elbow replacement first undergo placement of an indwelling auxiliary or infraclavicular catheter for postoperative pain control. General anesthesia is then administered for the procedure. The surgical technique is specific to the chosen implant design. When a linked implant is to be used, most surgeons advocate the posterior triceps–sparing Mayo (Bryan-Morrey) approach, which preserves the continuity of the triceps and anconeus by the subperiosteal elevation of the triceps insertion [5,21]. A posterolateral Kocher approach is most often used for unlinked implant surgery. At our institution, tourniquet time averages 2 hours for primary linked TEA [15,27,28]. Patients who have undergone linked TEA are splinted in extension for 24 to 36 hours, and thereafter active range of motion exercises are begun. Rehabilitation of unlinked implants is more patient specific, depending on the integrity of the repaired or reconstructed ligaments. The average postoperative hospital stay at our institution is 2 days. Many patients are discharged with the indwelling axillary catheter in place with the local anesthetic delivered by a disposable vacuum reservoir pump for five days. This gives the patient prolonged pain relief after surgery.
Most patients require little or no supervised physical therapy after semiconstrained TEA. Patients are encouraged to move the elbow through a range of motion and participate in activities of daily living, as dictated by their pain levels in the early postoperative period. Strict guidelines on lifting capacity are emphasized during preoperative decision making and during postoperative visits. Currently, our institution allows lifting of up to 0.9 kg (2 lb) repeatedly and not more than 4.5 kg (10 lb) during a single event. Sports activities such as golf and tennis are not allowed after TEA. A patient’s inability to commit to these activity restrictions is a contraindication for surgery.
Results
Direct comparison of outcome studies among the various linked and unlinked TEA implants is an arduous task. Given the many reported methods to score extremity function, patient satisfaction, and long-term radiographic analysis, comparing one study to another is difficult. Certain trends are not in dispute, however. The improved cementation techniques and improved implant designs of the past 10 to 15 years have other encouraging reports show a trend that the success rate of TEA for rheumatoid arthritis approaches that following total knee arthroplasty [5,12,18,20].Owing to the expanded indications available to the semiconstrained linked prosthesis, use of these implants has increased in the past decade over use of unlinked implants.
Recently, several studies have shown improved outcomes in elderly patients (>70 years) undergoing primary linked TEA compared with patients having undergone standard fracture fixation techniques for complex intra-articular fractures of the distal humerus. This improvement is arguably enough so as to recommend TEA as the procedure of choice in elderly patients [1,2,19].Revision TEA for implant loosening, polyethylene wear, implant failure, and periprosthetic fractures can result in satisfactory outcomes in a majority of patients [5]. At our institution, we perform nearly equal numbers of primary and revision TEA procedures each year.
Conclusions
Total elbow arthroplasty (TEA) has proven to be a reliable joint replacement procedure that has a high degree of patient satisfaction. The long-term functional and implant survival scores rival those of total knee arthroplasty. Despite these favorable outcomes, few patients with disabling elbow degenerative conditions have TEA recommended to them as an alternative procedure by rheumatologists, physiatrists, or orthopedists. This article reviews the history, current concepts, and future of TEA.
References
- Armstrong AD, Yamaguchi K (2004) Total elbow anthroplasty and distal humerus elbow fractures. Hand Clin 20: 475-483.
- Hastings H II, Theng CS (2003) Total elbow replacement for distal humerus fractures and traumatic deformity: results and complications of semiconstrained implants and design rationale for the Discovery Elbow System. Am J Orthop 32 Suppl: 20-28.
- Wright TW, Wong AM, Jaffe R (2000) Functional outcome comparison of semiconstrained and unconstrained total elbow arthroplasties. J Shoulder Elbow Surg 9: 524-531.
- Coonrad RW (1982) History of total elbow arthroplasty. In: Inglis AE, editor. Symposium on total joint replacement of the upper extremity. St. Louis: Mosby p. 75-90.
- Gill DRJ, Morrey BF, Adams RA (2000) Total elbow arthroplasty in patients with rheumatoid arthritis. In: Morrey BF, editor. The elbow and its disorders. 3rd ed. Philadelphia: Saunders p. 631-639.
- Hurri L, Pulkki T, Vainio K (1964) Arthroplasty of the elbow in rheumatoid arthritis. Acta Chir Scand 127: 459-465.
- Mellen RH, Phallen GS (1947) Arthroplasty of the elbow by replacement of the distal portion of the humerus with an acrylic prosthesis. J Bone Joint Surg 29: 348-353.
- Morrey BF (1991) Semi-constrained total elbow arthroplasty. New York: Churchill Livingston.
- Dee R (1972) Total replacement arthroplasty of the elbow for rheumatoid arthritis. J Bone Joint Surg Br 54: 88-95.
- Mansat P (2001) Surgical treatment of the rheumatoid elbow. Joint Bone Spine 68: 198-210.
- Morrey BF, Bryan RS, Dobyns JH, Linscheid RL (1981) Total elbow arthroplasty: a five-year experience at the Mayo Clinic. J Bone Joint Surg Am 63: 1050-1063.
- Rahme H, Jacobsen MB, Salomonsson B (2001) The Swedish Elbow Arthroplasty Register and the Swedish Shoulder Arthroplasty Register: two new Swedish arthroplasty registers. Acta Orthop Scand 72: 107-112.
- Barr JS, Eaton RG (1965) Elbow reconstruction with a new prosthesis to replace the distal end of the humerus: a case report. J Bone Joint Surg Am 47: 1408-1413.
- Chafik D, Lee TQ, Gupta R (2004) Total elbow arthroplasty: current indications, factors affecting outcomes, and followup results. Am J Orthop 33: 496-503.
- Ewald FC, Simmons Jr ED, Sullivan JA, Thomas WH, Scott RD, et al. Capitellocondylar total elbow replacement in rheumatoid arthritis: long-term results. J Bone Joint Surg Am 75: 498-507.
- Goldberg VM, Figgie HE III, Inglis AE, Figgie MP (1988) Total elbow arthroplasty. J Bone Joint Surg Am 70: 778-783.
- Gschwend N, Scheier NH, Baehler AR (1999) Long-term results of the GSB III elbow arthroplasty. J Bone Joint Surg Br 81: 1005-1012.
- Little CP, Graham AJ, Carr AJ (2005) Total elbow arthroplasty: a systematic review of the literature in the English language until the end of 2003. J Bone Joint Surg Br 87: 437-444.
- Morrey BF, Askew LJ, Chao EY (1981) A biomechanical study of normal functional elbow motion. J Bone Joint Surg Am 63: 872-877.
- Van der Lugt JC, Rozing PM (2004) Systematic review of primary total elbow prostheses used for the rheumatoid elbow. Clin Rheumatol 23: 291-298.
- Gill DR, Morrey BF (1998) The Coonrad-Morrey total elbow arthroplasty in patients who have rheumatoid arthritis: a ten to fifteen-year follow-up study. J Bone Joint Surg Am 80: 1327-1335.
- Hildebrand KA, Patterson SD, Regan WD, MacDermid JC, King GJ (2000) Functional outcome of semiconstrained total elbow arthroplasty. J Bone Joint Surg Am 82: 1379-1386.
- King GJ (2002) New frontiers in elbow reconstruction: total elbow arthroplasty. Instr Course Lect 51: 43-51.
- Kraay MJ, Figgie MP, Inglis AE, Wolfe SW, Ranawat CS (1994) Primary semiconstrained total elbow arthroplasty: survival analysis of 113 consecutive cases. J Bone Joint Surg Br 76: 636-640.
- Morrey BF, Adams RA (1992) Semiconstrained arthroplasty for the treatment of rheumatoid arthritis of the elbow. J Bone Joint Surg Am 74: 479-490.
- Madsen F, Gudmundson GH, Sojbjerg JO, Sneppen O (1989) The Pritchard Mark II elbow prosthesis in rheumatoid arthritis. Acta Orthop Scand 60: 249-253.
- Rauhaniemi J, Tiusanen H, Kyro A (2006) Kudo total elbow arthroplasty in rheumatoid arthritis: clinical and radiological results. J Hand Surg 31: 162-167.
- Van der Lugt JC, Geskus RB, Rozing PM (2004) Primary Souter- Strathclyde total elbow prosthesis in rheumatoid arthritis. J Bone Joint Surg Am 86: 465-473.
- Van der Lugt JC, Geskus RB, Rozing PM (2005) Limited influence of prosthetic position on aseptic loosening of elbow replacements: 125 elbows followed for an average period of 5.6 years. Acta Orthop 76: 654-661.
Citation: Saccomanni B (2026) Past, Present and Future of Tea (Total Elbow Arthroplasty). J Emerg Med Trauma Surg Care 12: 077.
Copyright: © 2026 Bernardino Saccomanni, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.

