
Self-Inserted Rectal Foreign Bodies, Still a Challenging Diagnosis
*Corresponding Author(s):
Carlos J RoldanDepartment Of Emergency Medicine, Memorial Hermann Hospital, Texas Medical Center, Anderson Cancer Center - Texas Medical Center, Lyndon Baines Johnson General Hospital, The University Of Texas Health Science Center At Houston, Houston, Texas, United States
Tel:+1 7135007933,
Email:croldan@mdanderson.org, carlos.j.roldan@uth.tmc.edu
Abstract
Background: A patient’s medical history is the most valuable diagnostic tool a healthcare provider uses when determining treatment. The accuracy of a diagnosis and treatment plan can be affected by the patient’s unwillingness to disclose intimate information. Numerous clinical scenarios seem to explain this behavior. The presence of a Retained Self-Inserted Rectal Foreign Body (RSIRFB) is not an unusual finding in the Emergency Department (ED) setting. Still, it can present a diagnostic challenge even to seasoned clinicians.
Case report: A healthy man presented to our ED complaining of “constipation”. The patient had visited another ED the day before, after suffering a syncopal episode while sitting on the toilet, and had been discharged after a negative workup. He did not disclose that information. An abdominal single view radiograph revealed a rectal foreign body, which explained the reasons for both ED visits.
Discussion: Patient’s denial or misleading information makes of a RSIRFB a challenging diagnosis. It might be suspected in patients with vasovagal syncope associated with defecation, rectal or abdominal pain, bleeding from the rectum, an inability to have a bowel movement, and rectal mucous leakage, all in the context of otherwise healthy individuals or in presence of history inconsistencies.
Keywords
INTRODUCTION
Physical diagnosis is traditionally based on history taking and a physical exam. Inaccuracy in the information provided by patients can be a significant hindrance to correct diagnosis. Embarrassment and fear of public exposure are among the known reasons for this behavior. A RSIRFB clearly exemplifies such a situation. The literature about RSIRFBs is mostly anecdotal; however, it has been described in the medical field for many years [1]. The occurrence of RSIRFBs has been reported in patients of all backgrounds and ages; however, it is more common in men in their 30s and 40s [2]. The incidence of RSIRFBs varies according to region; it is presumed to be uncommon in Asia and most common in Eastern Europe [3]. Whereas rectal foreign bodies can occur as a result of sexual abuse, drug packing, physical assault, and mental illness, RSIRFBs more generally occur in the context of sexual activities. Failed self-removal attempts and reluctance to state the true nature of the visit are common contributors for delays in diagnosis and for the resulting increased morbidity. All RSIRFBs should be treated as potentially harmful. Overall, the morbidity correlates with the size, shape, nature, and texture of the inserted object.
CASE REPORT
A 43-year-old man with no past medical history presented to our Emergency Department (ED) complaining of constipation. His last bowel movement had occurred two days before. He also reported feeling bloated. He stated he didn’t have nausea, vomiting or pain. He denied using tobacco, alcohol, or illicit drugs. His household included two children and a wife. He denied prior surgeries or taking any medications. His vital signs and his physical exam including his rectal exam were within normal limits. In order to visualize his fecal content, single view abdominal radiography was requested.
His medical records revealed that he had visited another ED the day before as a result of a syncopal episode while sitting on the toilet. He had negative results for all evaluations at the previous ED, including computed tomography of the brain, electrocardiography, cardiac enzyme levels, chest radiography, and basic laboratory values, and was discharged. The patient did not provide this information upon presenting to our ED. Once confronted, he confirmed it but offered no additional details.
A final diagnosis became clear based on the Kidney-Ureter-Bladder (KUB) radiograph (Figure 1). A self-inserted foreign body had been present in his rectum for more than 30 hours. The patient declined to comment about it and requested that the diagnosis and treatment not be disclosed to his spouse and family. The patient was sedated and an 8.5-inch silicone phallic-shaped device was removed rectally in the ED. The patient was discharged with no further complaints after six hours of observation. In retrospect, the final diagnosis should have been suspected in both ED visits based on the clinical presentation and history gaps, including the nondisclosure of prior visit.
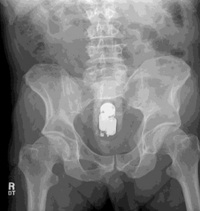 Figure 1: Upright abdominal radiograph.
Figure 1: Upright abdominal radiograph.
DISCUSSION
During the medical history-taking process, ED patients can be sensitive to their unfamiliarity with the physician and be reticent to disclose certain types of personal information. The disclosure or lack of disclosure, of intimate information affects the accuracy of the interview [4]. A 2004 WebMD survey of 1,500 respondents found that 45% admitted to lying to their physicians. The primary reason given was to avoid judgment. Most of them lied about following doctors’ orders, diet, exercise, smoking, and/or alcohol or illicit drug consumption [5]. In addition, matters of legal concern, secondary gain, drug seeking, social stigmatization, and embarrassment were also commonly perceived justifications for withholding and denying medical information.
Regarding RSIRFBs, in addition to sexually related, they are a common result of intentional concealment (body smuggling and body packing) of cocaine and other illegal substances [6,7]. When unable to expel the rectal foreign body, patients attempt different maneuvers before seeking medical help. Self-directed removal strategies include digital removal, straining and bowel movement induction with laxatives and suppositories. As patients can be initially asymptomatic, they may develop rectal or abdominal pain, bleeding from the rectum, an inability to pass stool, and rectal mucous leakage. These symptoms are of more clinical significance in the context of otherwise healthy individuals or history inconsistencies [8,9]. More surprising, even in advanced cases of bowel perforation with peritonitis, some patients are still reluctant to release such personal information.
Regarding vasovagal syncope, it is considered to be a reflex characterized by a transient loss of neural control of circulation. The exact anatomic and physiologic nature of this reflex remains uncertain [10]. The most common triggers are central (in response to emotional stimuli), postural (associated with an upright position and external maneuvers), and situational (in response to specific stimuli) [11]. Postural vasovagal syncope is by far the most common type. Paradoxical impulses from thoracic hypovolemia, splanchnic blood pooling, and increased ventilation are conducted by vagal afferents to the brain stem. The response is transient vagal stimulation of the heart and widespread sympathetic withdrawal [12]. Postural vasovagal syncope is extremely rare in otherwise healthy and asymptomatic individuals. Similarly, a vasovagal episode during defecation in a healthy individual is such an unusual event that an RSIRFB should be considered in the differential diagnosis.
Constipation, although commonly seen in the ED, is diagnosed on the basis of symptoms. A more precise and accurate characterization of the underlying mechanism(s) requires physiological tests of colorectal function [13]. The Rome III Criteria for diagnosing functional constipation include symptoms of straining in at least 25% of the defecations and fewer than three defecations per week during the last 3 months, with symptom onset at least 6 months before the diagnosis [14]. A radiograph of the abdomen is commonly used to complement the clinical history. However, due to inter-observer variability in radiological assessment, it is considered to have poor correlation with colonic transit [15].
CONCLUSION
Abdominal radiographs may not be a reliable method to assess for fecal loading in constipation. Therefore, the clinical usefulness of abdominal radiographs in the ED prevails in ruling out other pathologies. In the clinical practice of emergency medicine, abdominal radiographs have been an invaluable diagnostic tool, able to demonstrate acute fecal retention and incidental findings such as RSIRFB in patients complaining of constipation. Patients might be suspected of providing intentional inaccuracies in the presence of inconsistencies in their history and lack of clinical correlation. Vasovagal syncope associated with defecation, rectal or abdominal pain, bleeding from the rectum, an inability to have a bowel movement, and rectal mucous leakage, all in the context of otherwise healthy individuals or history inconsistencies, should raise the suspicion for retained RSIRFBs.
REFERENCES
- Rosser C (1929) Colonic foreign bodies. JAMA 39: 368-369.
- Clarke DL, Buccimazza I, Anderson FA, Thomson SR (2005) Colorectal foreign bodies. Colorectal Dis 7: 98.
- Akhtar MA, Arora PK (2009) Case of unusual foreign body in the rectum. Saudi J Gastroenterol 15: 131-132.
- Palmieri J, Stern T (2009) Lies in the doctor-patient relationship. Prim Care Companion J Clin Psych 11: 163-168.
- Editorial Survey on WebMD Health (2014) “Why Do You Lie to Your Doctor?”
- Birnbach DJ, Browne IM, Kim A, Stein DJ, Thys DM (2001) Identification of polysubstance abuse in the parturient. Br J Anaesth 87: 488-490.
- Hollander JE, Henry TD (2006) Evaluation and management of the patient who has cocaine-associated chest pain. Cardiol Clin 24: 103-114.
- Ji R-H, Codina-Cazador A, Ruiz B, Sirvent JM, Roig J, et al. (2007) Management of foreign bodies in the rectum. Colorectal Dis 9: 543-548.
- Goldberg JE, Steele SR (2010) Rectal Foreign Bodies. Surg Clin N Am 90: 173-184.
- Jardine DL (2013) Vasovagal syncope: new physiologic insights. Cardiol Clin 31: 75-87.
- Colman N, Nahm K, van Dijk JG, Reitsma JB, Wieling, Wet al.(2004) Diagnostic value of history taking in reflex syncope. Clin Auton Res 2004; 14: 37-44.
- Thorén P (1979) The role of cardiac vagal C-fibres in cardiovascular control. Rev Physiol Biochem Pharmacol 86: 1-94.
- Rao SS, Ozturk R, Laine L (2005) Clinical utility of diagnostic tests for constipation in adults: a systematic review. Am J Gastroenterol 100: 1605-1615.
- Rao SSC (2009) Approach to the Patient with Constipation. Principles of clinical gastroenterology. Wiley-Blackwell, Oxford, UK.
- Cowlam S, Vinayagam R, Khan U, Marsden S, Minty I et al. (2008) Blinded comparison of fecal loading on plain radiography versus radio-opaque marker transit studies in the assessment of constipation. Clin Radiol 63: 1326-1331.
Citation: Roldan CJ, Bilow RM (2015) Self-Inserted Rectal Foreign Bodies, Still a Challenging Diagnosis. J Emerg Med Trauma Surg Care 2: 008.
Copyright: © 2015 Carlos J Roldan, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.

