
A Case of Ocular Ischaemic Syndrome Associated with Choroidal Folds
*Corresponding Author(s):
Fatma Selin KayaBasaksehir Cam Ve Sakura City Hospital, Ophthalmology Department, Basaksehir, 34480, Istanbul, Turkey
Tel:+90 2129096000,
Email:fatselink@gmail.com
Abstract
A 58 year-old male patient presented with fluctuating vision in right eye. Dilated fundus examination on presentation showed wavy choroidal folds and cotton wool spots in the posterior pole of right eye. Fundus fluorescein angiogram demonstrated prolonged arm-to-retina circulation time and a patchy choroidal filling pattern in the same eye. The carotid evaluation revealed complete stenosis of the right internal carotid artery. We report a case showing choroidal folds can be linked with Ocular Ischaemic Syndrome (OIS) and propose a possible pathogenic mechanism for development of choroidal folds in OIS.
Introduction
Ocular involvement can be observed in carotid disease, and ocular symptoms may be the first sign of carotid artery stenosis [1]. Ocular Ischaemic Syndrome (OIS) is a rare condition, which is caused by ocular hypoperfusion associated with stenosis of the Internal Carotid Artery (ICA) or the common carotid artery [2].
The most common anterior characteristics include iris neovascularization, iridocyclitis, asymmetric cataract, iris atrophy. The main findings of posterior segment are perifoveal telangiectasias, dilated retinal veins, mid-peripheral retinal hemorrhages, microaneurysms, neovascularization at the optic disk and in the retina, a cherry-red spot, cotton-wool spots, vitreous hemorrhage [3].
Although choroidal folds can be seen in association with various conditions [4], OIS is rarely associated with choroidal folds. Therefore, we report a case of OIS with a rare finding of choroidal folds and discuss possible pathogenic mechanisms for development of choroidal folds in OIS.
Case Report
A 58-year-old man presented at our hospital with fluctuating vision in the right eye. Best Corrected Visual Acuity (BCVA) was 0.8 OD and 1.0 OS. The intraocular pressure (IOP) was 16mmHg in the right eye and 22 mmHg in the left eye. In addition, no iris rubeosis, inflammation or relative afferent pupillary defect was observed in either eye. Fundus examination of the right eye demonstrated severe retinal vascular abnormalities with cotton wool spots, choriodal folds and optic disc pallor (Figure 1). At presentation, the optic disk of the right eye had mild edema which was evident on Fluorescein Angiography (FFA) as optic disk staining (Figure 2). FFA showed multiple sites of non-perfusion area and delayed arteriolar filling, suggestive of ocular ischaemie (Figure 3). Erythrocyte Sedimentation Rate (ESR), and C-Reactive Protein (CRP) were within normal limits. The laboratory blood test findings showed that the Lactate Dehydrogenase was 275U/L and the total cholesterol level was 290 mg/dl, suggesting that they were elevated. Orbital magnetic resonance imaging excluded orbital mass. In the present case, retinal cotton wool exudates and prolonged arterial filling in the posterior pole suggested a decrease in ocular blood flow. He immediately started conservative treatment with anti-platelet drugs. In order to evaluate the carotid artery stenosis, a carotid ultrasound was performed, and it showed subtotal occlusion of the right ICA. Subsequently, we performed Magnetic resonance (MR) angiography and MR angiography revealed complete total occlusion of the right ICA and 50% stenosis of the left ICA. We referred the patient to the department of vascular surgery, where it was determined that ICA stenting was necessary for the stenosis.
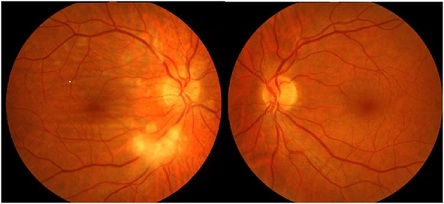 Figure 1: Fundus photographs of the right and left eye. Fundus photograph of the right eye showed soft exudates and choroidal folds.
Figure 1: Fundus photographs of the right and left eye. Fundus photograph of the right eye showed soft exudates and choroidal folds.
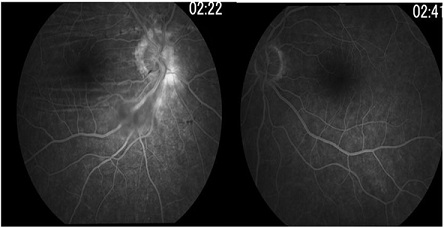 Figure 2: Fundus fluorescein angiography of the right and left eye: hyperfluorescence at the disc margin of the right optic nerve and choroidal folds in the right eye are seen.
Figure 2: Fundus fluorescein angiography of the right and left eye: hyperfluorescence at the disc margin of the right optic nerve and choroidal folds in the right eye are seen.
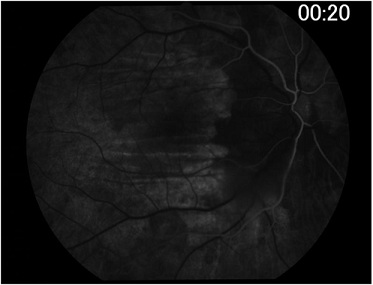 Figure 3: Fundus fluorescein angiography image taken at 20 s (arterial phase) demonstrated prolonged arm-to-retina circulation time and a patchy choroidal filling pattern.
Figure 3: Fundus fluorescein angiography image taken at 20 s (arterial phase) demonstrated prolonged arm-to-retina circulation time and a patchy choroidal filling pattern.
Discussion
Ocular ischemic syndrome is a serious condition that generally causes visual loss and ocular angina. The current case had right OIS due to complete occlusion of the right ICA. The features of OIS in this patient include ocular angina, cotton wool spots and choroidal folds.
Our patient had ocular pain at presentation in the absence of neovascular glaucoma which might suggest ischemia was the likely cause. Normal ESR, CRP and absent suggestive history/clinical features excluded giant cell arteritis in present patient.
Choroidal folds are undulations located in the retinal pigment epithelium, Bruch's membrane, and inner choroid. They are generally associated with orbital disease, choroidal tumors, ocular hypotony, scleritis, ocular inflammation and papilledema [4]. Among the mechanisms which are responsible for choroidal fold formation seen with OIS, a few potential mechanisms can be considered. Ocular hypony might be one of the mechanisms associated with choroidal fold. However, normal intraocular pressure value excluded ocular hypotony in our patient. The intraocular pressure is usually less than 6 mm of Hg in choroidal folds related to hypotony [5]. The second mechanism associated with the choroidal folds in the present case would be the, acute congestion of ocular tissues as a result of decreased blood flow. Choroidal fold formation caused by congestion of the choroid is described previously. In cases with scleritis, acute Vogt-Koyanagi-Harada disease, and papilledema, increased choroidal thickness may be related to choroidal folds [6,7]. Any stenoses of the ICA affect both retinal and choroidal blood flows. Carotid studies revealed complete stenosis of the right internal carotid artery and 50% stenosis of the left internal carotid artery in the present case. Therefore we suggest that sudden occlusion of ICA may result in congestion of the choroid leading to choroidal folds. Factors that cause the normal expansion of Bruch's membrane to shorten are considered to contribute to the development of choroidal folds. Congestion of choroid compressing the Bruch's membrane, followed capillary leakage to the intersistial space results from the total occlusion of ICA (Figure 4). Congestion of the choroid and adhesions to Bruch's membrane are probably prerequisites for folds to form in current case.
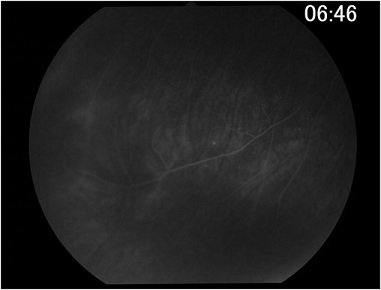 Figure 4: Late phase fundus fluorescein angiography showed peripheral vascular leakage in the right eye.
Figure 4: Late phase fundus fluorescein angiography showed peripheral vascular leakage in the right eye.
We reported a patient with total internal carotid artery obstruction who presented with choroidal folds and soft exudates. Congestion of the choroid due to sudden decrease of ocular blood flow and adhesions to Bruch's membrane are considered to contribute to the development of choroidal folds in this case. As clinical diagnosis might be challenging, physicians should be aware of the rare ocular manifestations of this potentially fatal condition.
Funding
The authors declare that they have not received grant support or research funding and they do not have any proprietary interests in the materials described in the article.
Declarations of Interest
None
References
- Dugan JD Jr, Green WR (1991) Ophthalmologic manifestations of carotid occlusive disease. Eye (Lond) 5: 226-238.
- Mendrinos E, Machinis TG, Pournaras CJ (2010) Ocular ischemic syndrome. Surv Ophthalmol 55: 2-34.
- Brown GC, Magargal LE (1988) The ocular ischemic syndrome: clinical, fluorescein angiographic and carotid angiographic features. Int Opththalmol 11: 239-251.
- Agrawal M, Tripathy K (2022) Choroidal Folds. In: StatPearls Treasure Island (FL): StatPearls Publishing.
- Bullock JD, Egbert PR (1974) Experimental choroidal folds. Am J Ophthalmol 78: 618-623.
- Benson WE (1988) Posterior scleritis. Surv Ophthalmol 32: 297-316.
- Zhao C, Zhang M, Wen X, Dong F, Han B, et al. (2009) Choroidal folds in acute Vogt-Koyanagi-Harada disease. Ocul Immunol Inflamm 17: 282-288.
Citation: Kaya FS, Kasapoglu E, Onur U, Iscan Ö, Örüm Ö (2022) A Case of Ocular Ischaemic Syndrome Associated with Choroidal Folds. J Ophthalmic Clin Res 9: 093.
Copyright: © 2022 Fatma Selin Kaya, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.

