
A Case of Unilateral Optic Neuritis in a 13Year Old Boy
*Corresponding Author(s):
Anushree GuptaDr Radhakrishnan Government Medical College, Hamirpur, Himachal Pradesh, India
Email:anushree0612@gmail.com
Abstract
It is widely known that in children, optic neuritis usually occur following a febrile illness, tend to affect both eyes and frequently associated with swollen discs with good visual outcomes. We report a case of a13 year old boy who presented with 10 days history of blurred vision in right eye and pain with eye movements. Slit lamp examination and fundoscopy was normal. Investigative workup for infectious, autoimmune and neoplastic was negative. Magnetic resonance imaging (MRI) of the brain and orbit revealed swelling of the retrobulbar intra-orbital segment of the optic nerve with a high T2 signal. A diagnosis of retrobulbar optic neuritis was made and patient was started on intravenous methylprednisolone for 3 days, followed by oral prednisolone for 14 days. He had excellent visual recovery and remained asymptomatic for 1 year.
Keywords
Childhood; Optic neuritis, Unilateral
ABBREVIATIONS
MRI: Magnetic Resonance Imaging
MS: Multiple Sclerosis
NMO: Neuromyelitis Optica
ADEM: Acute Disseminated Encephalomyelitis
INTRODUCTION
Optic neuritis refers to inflammation of the optic nerve. It is referred to as papillitis when the optic disc is swollen and retrobulbar neuritis when the disc appears normal. The majority of patients are between the ages of 20 and 50 years. Women are affected more commonly than men. The clinical presentation of this pathology usually includes sudden loss of visual acuity which may be unilateral or bilateral, visual field defects, painful eye movements, dyschromatopsia and a relative afferent pupillary defect [1,2].
CASE REPORT
A 13-year-old boy presented in Ophthalmology OPD at Dr. Radhakrishnan Government Medical College, Hamirpur, Himachal Pradesh with blurring of vision in his right eye for the past 10 days. Patient also complained of pain during eye movements. The boy and his family were natives to this place. There was no history of preceding febrile illness. There was no significant family history.
On examination, right visual acuity was 6/18 with no improvement with pinhole and 6/6 in the left eye. Colour vision (Ishihara) at presentation was severely impaired in the right eye and normal in the left eye. Ocular movements were full range but associated with pain.
No conjunctival congestion or lid swelling was noted. A relative afferent pupillary defect (RAPD) was noted in the right eye. Anterior segment of both the eyes was normal. Funduscopy was normal (Figure 1 and 2). Rest of systemic and neurological examination were normal.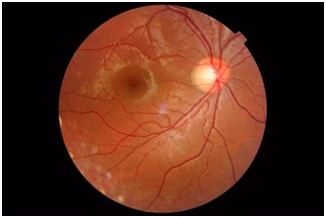
Figure 1: Fundus photograph of Right eye with retrobulbar optic neuritis.
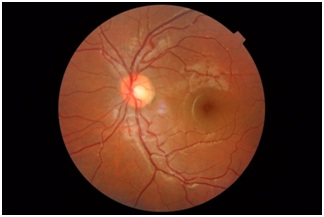 Figure 2: Fundus photograph of normal left eye.
Figure 2: Fundus photograph of normal left eye.
Chest X ray and Mantoux skin test was negative. Blood inflammatory markers were normal and blood analysis was negative for infectious pathology. Magnetic Resonance Imaging (MRI) of the brain and orbit revealed swelling of the retrobulbar intra-orbital segment of the optic nerve with a high T2 signal (Figure 3 and 4). Brain parenchyma and left optic nerve were normal. A diagnosis of isolated unilateral retrobulbar optic neuritis was made.
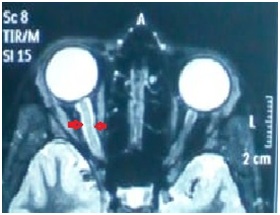 Figure 3: Axial T 2 MRI scan showing swelling of retrobulbar intraorbital segment of optic nerve of the right eye.
Figure 3: Axial T 2 MRI scan showing swelling of retrobulbar intraorbital segment of optic nerve of the right eye.
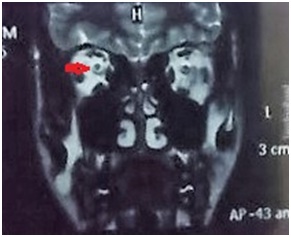 Figure 4: Coronal T2 MRI scan showing retrobulbar optic nerve swelling of the right eye.
Figure 4: Coronal T2 MRI scan showing retrobulbar optic nerve swelling of the right eye.
He was started on 250mg 4th hourly Intravenous Methyl prednisolone for 3 days followed by oral steroids 40mg for 11 days with 3 day tapering in consultation with paediatrician and physician.
At 2 weeks patient’s vision in the right eye had improved to 6/6 and colour vision test using Ishihara plates was normal.
At 1 month post episode of optic neuritis, his right eye optic disc showed mild temporal pallor. At 1 year follow up, he has maintained his vision and his neurological examination is normal.
DISCUSSION
Optic neuritis affects children less commonly than adults. The presentation is typically bilateral and frequently has optic nerve head swelling. The prognosis is generally good. Pediatric optic neuritis may occur following infection or vaccination, or in association with a systemic demyelinating diseases such as Multiple Sclerosis (MS), Neuromyelitis Optica (NMO) or initial manifestation of Acute Disseminated Encephalomyelitis (ADEM) [3,4].
Children with monosymptomatic optic neuritis and an abnormal brain MRI have a higher risk for multiple sclerosis. Neuromyelitis Optica (NMO) is a central nervous disorder with features of optic neuritis, myelitis, as well as brainstem and cerebral signs and is further categorized by AQP4-IgG status .ADEM is a polyfocal CNS disease with encephalopathy, usually occurring in young children [5].
A Study done in paediatric optic neuritis in Indian population found bilateral presentation more common and association with MS was low as compared to adults. Papillitis was more frequent than retrobulbar neuritis and prognosis was good [6]. Systemic steroids were found to benefit paediatric patients with optic neuritis in another study in India [7].
Initial assessment should be directed toward ruling out those diseases for which delay in treatment can result in permanent vision loss or other neurologic impairment. The following blood tests are recommended such as Complete Blood Count (CBC), Anti-Neutrophil Cytoplasmic Antibody (ANCA), Anti-Nuclear Antibody (ANA), Angiotensin-Converting Enzyme (ACE), and anti-AQP4-IgG levels. Chest x-ray and Mantoux test may be done in case of suspicion of pulmonary disease.
Other diagnostic tests include MRI of the brain and orbits with fat suppression and gadolinium enhancement, Cerebrospinal Fluid (CSF) analysis, Optical Coherence Tomography (OCT) and Visual Evoked Potential (VEP) testing [8].
Optic Neuritis Treatment Trial (ONTT). This was a multicenter trial supported by the National Eye Institute that assessed the benefit of corticosteroid treatment and investigated the relation between optic neuritis and multiple sclerosis (MS). It was found that monosymptomatic patients in the intravenous methylprednisolone group had a reduced rate of development of MS during the first 2years of follow-up. Brain MRI is the most powerful predictor of subsequent MS risk in monosymptomatic patient. The presence of one or more white matter lesions was associated with a 56% risk of MS after 10years, while the risk was only 22% if the MRI results were normal [9]. This study, however, did not include pediatric patients.
The pathogenesis of pediatric optic neuritis is not well understood. The Pediatric Optic Neuritis Prospective Outcomes Study is being done to study this rare disease in children and provide knowledge regarding the etiology, management and prognosis of optic neuritis in children [10].
Our patient presented with unilateral retrobulbar optic neuritis with no lesion in brain. His systemic and neurological examination was normal. The prognosis is relatively good in such children. Our patient promptly responded to systemic steroids and had excellent visual recovery.
There are no clear guidelines regarding treatment in paediatric population with isolated optic neuritis without central nervous involvement. Some suggest monitoring as vision usually recovers in 1 month. Treatment in the pediatric population consists of 30 mg/kg per day intravenous methylprednisolone, maximum 1 g daily, for 3-5 days followed by oral corticosteroid taper over ( 2-4) week. Treatment with systemic steroids helps in quicker visual recovery although they do not alter the final visual outcome [11-13].
CONCLUSION
Optic neuritis in children presents with different clinical manifestations than in adults. The risk of evolving MS is reported to be less than in adults. Although bilateral, painless papillitis is more frequent but can also present as isolated, unilateral retrobulbar as in our case. It is important to rule out any serious neurological disorder through a thorough history, physical examination, and imaging. Neuroimaging should be done to rule out any demyelinating lesion or any intracranial pathology. The pathogenesis of pediatric optic neuritis is not well understood. Prospective studies are required to enlighten us regarding diagnosis and management in cases of paediatric optic neuritis.
REFERENCES
- Yanoff F, Duker JS (2014) Inflammatory Optic Neuropathy. Ophthalmology, 4th
- Yeh EA, Graves JS, Benson LA, Wassmer E, Waldman A (2016) Pediatric optic neuritis. Neurology 87: 53-58.
- Singh D, Phuljhele S, Sharma R, Saxena R, Sharma P, et al. (2017) Clinical spectrum of pediatric optic neuritis in indian children. Ophthalmol Open J 2: 20-26.
- Rafael José Pérez-Cambrodí, Aránzazu Gómez-Hurtado Cubillana, María L. Merino-Suárez, David P. Piñero-Llorens, Carlos Laria-Ochaita (2014) Optic neuritis in pediatric population: Areview in current tendencies of diagnosis and management. J Optom 7: 125-130.
- Chang MY, Pineles SL (2017) Pediatric Optic Neuritis. Semin Pediatr Neurol 24: 122-128.
- Khadse R, Ravindran M, Pawar N, Maharajan P, Rengappa R (2017) Clinical profile and neuroimaging in pediatric optic neuritis in Indian population: A case series. Indian J Ophthalmol 65: 242-245.
- Kumar KVP, Chiranjeevi P (2017) Optic neuritis in indian children: a one year followup study . Opth Clin ther 1: 3-5.
- Borchert M, Liu GT, Pineles S, Waldman AT (2017) Pediatric Optic Neuritis: What Is New. J Neuroophthalmol 37: 14-22.
- Cleary PA, Beck RW, Anderson MM, Kenny DJ, Backlund J, et al. (1993) Design, methods and conduct of the Optic Neuritis Treatment Trial. Control Clin Trials 14: 123-142.
- Pineles SL, Liu GT, Waldman AT, Lazar E, Kupersmith MJ, et al. (2016) Pediatric Optic Neuritis Prospective Outcomes Study. J Neuroophthalmol 36: 115-117.
- Brady KM, Brar AS, Lee AG, Coats DK, Paysse EA, et al. (1999) Optic neuritis in children: clinical features and visual outcome. J AAPOS 3: 98-103.
- Menon V, Saxena R, Misra R, Phuljhele S (2011) Management of optic neuritis. Indian J Ophthalmol 59: 117-22.
- Bonhomie GR, Mitchell EB (2012) Treatment of Pediatric Optic Neuritis. Curr Treat Options Neurol. 14: 93-102.
Citation: Gupta A (2019) A Case of Unilateral Optic Neuritis in a 13Year Old Boy. J Ophthalmic Clin Res 6: 055.
Copyright: © 2019 Anushree Gupta, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.

