
Bilateral Orbital Extension of Acute Myeloid Leukemia Masquerading as Burkitt Lymphoma: A Case Report
*Corresponding Author(s):
Caroline MvilongoYaounde Central Hospital, Department Of Ophthalmology, Faculty Of Medicine And Biomedical Sciences, University Of Yaoundé, PO Box 1364, Yaoundé, Cameroon
Tel:+237 699324796; +237 670312700,
Email:carolinemvilongo@yahoo.fr
Abstract
We report the case of a three-year-old girl with left sided facial swelling and proptosis as the initial presentation of bilateral orbit involving Acute Myeloid Leukemia (AML) in Cameroon. Despite being less typical in childhood, AML is the most common leukemia to cause orbital leukemic tumors. Solid extramedullary AML involves the orbit in 30% of cases and is bilateral in one third patients. Our patient responded well to two rounds of chemotherapy using aracytine, daunorubicine and filgrastim. Rapid diagnosis and systemic treatment, irrespective of systemic manifestations, is warranted to achieve the best possibility of long-term disease-free survival for patients with AML.
Keywords
Acute myelogenous leukemia; AML; Burkitt lymphoma; Cancer; Chemotherapy; Leukemia; Orbital extension
Introduction
Ocular and orbital tumors are the third most common extramedullary locations of acute leukemia after the meninges and testicles [1]. Up to 30% of solid tumours from extramedullary myeloid leukemia are found in the orbit [2]. Ocular and orbital tumors may be accompanied by hematologic abnormalities such as anemia, thrombocytopenia, or hyperviscosity syndrome. Isolated, pre-systemic, orbital and ocular involvement is also possible. These isolated lesions, termed myeloid sarcomas, are treated as central nervous system neoplasms; correct diagnosis is essential to their management. Misdiagnosis is common, but rapid treatment for Acute Myelogenous Leukemia (AML) may decrease the chance of developing systemic disease [3]. We report a case of a young girl with bilateral exophthalmos as the initial presentation of acute myeloid leukemia in Cameroon.
Case Report
A 3-year-old female presented with a one-and-a-half-month history of swelling of the left side face. Her past medical history was non-contributory. She was able to fix and follow with the right eye but had no light perception from the left eye. There was left sided proptosis, corneal decompensation, and chemosis. She had a firm indurated mass of the left side of her face (Figure 1A). There was deviation of her teeth to the left due to mass effect. Palpable lymphadenopathy was present in the left preauricular and cervical chains.
B-scan ultrasound revealed a left-sided heterogenous intra-orbital mass measuring 39.2 by 31.8 millimetres. Clinical suspicion for Burkitt’s lymphoma was high given the assumed unilateral nature of the lesion. Computed tomography of the brain and orbits revealed a homogenous hyperdense lesion occupying the paranasal sinuses and masticator spaces extending into both orbits and temporal regions, with a left sided exophthalmia (Figure 1B, 1C). The bilateral nature of the tumor raised suspicion for a leukemic infiltrate. A left anterior orbitotomy with biopsy was urgently performed, and she was admitted to the pediatric oncology service.
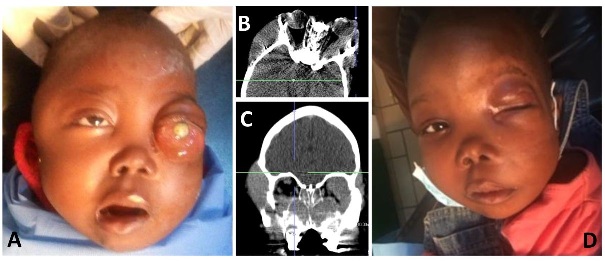 Figure 1: A) Clinical photo taken prior to starting chemotherapy. B) Axial computed tomography through the orbits showing a homogenous mass along the left lateral orbit with left proptosis. C) Coronal imaging showing infiltration of the paranasal sinuses with extension into both orbits. D) Clinical photo taken 7 months after completing chemotherapy showing improvement of mass effect.
Figure 1: A) Clinical photo taken prior to starting chemotherapy. B) Axial computed tomography through the orbits showing a homogenous mass along the left lateral orbit with left proptosis. C) Coronal imaging showing infiltration of the paranasal sinuses with extension into both orbits. D) Clinical photo taken 7 months after completing chemotherapy showing improvement of mass effect.
Histopathology revealed acute myeloid leukemia (Figure 2). She had an increased white blood cell count (51,300/mm3) with moderate anemia (8 g/dl). A peripheral blood smear showed numerous cells of the myeloid line. Cytology exam was consistent with AML Type 1. Renal function was normal. Two rounds of chemotherapy were performed using a combination of aracytine, daunorubicine, and filgrastim for 10 days each round. Blood transfusions were required for her anemia. She responded well to treatment with regression of the mass (Figure 1D). Unfortunately, the left eye remained blind.
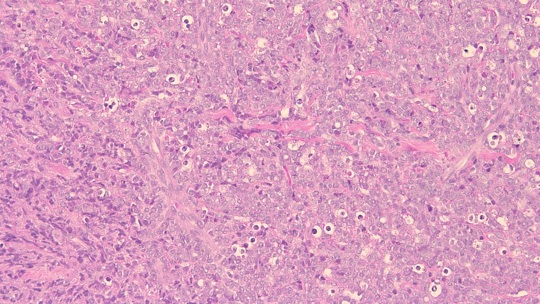 Figure 2: Hematoxylin and eosin stain of the biopsy (200x magnification) demonstrates fibroadipose tissue extensively involved by malignant neoplasm. Immunohistochemistry (not shown) demonstrates that the tumor cells are positive for CD34, TDT, myeloperoxidase, PAX-5, muramidase, CD117, CD68, MYC and BCL2. Ki-67 demonstrates a proliferation rate of virtually 100%. FISH studies show that the blasts have the t(8;21) karyotype.
Figure 2: Hematoxylin and eosin stain of the biopsy (200x magnification) demonstrates fibroadipose tissue extensively involved by malignant neoplasm. Immunohistochemistry (not shown) demonstrates that the tumor cells are positive for CD34, TDT, myeloperoxidase, PAX-5, muramidase, CD117, CD68, MYC and BCL2. Ki-67 demonstrates a proliferation rate of virtually 100%. FISH studies show that the blasts have the t(8;21) karyotype.
Discussion
Burkitt’s lymphoma is the most common tumor in some parts of Africa [4]. It was well established before the beginning of the Human Immunodeficiency Virus (HIV) epidemic, although it occurs more commonly in patients with HIV and has been associated with the Epstein Barr Virus. In the endemic form, it usually occurs in children and affects the orbit in 10 to 20% of cases. Therefore, Burkitt’s lymphoma should remain high on the differential when treating patients with rapidly progressive orbital masses in children. One may also consider rhabdomyosarcoma, metastatic neuroblastoma, Ewing’s sarcoma and a secondary extension of a retinoblastoma.
AML, conversely, is more common in patients older than 60 years and constitutes only 15 to 20% of childhood leukemia [5]. Yet, despite it being a less common cause of childhood leukemia overall, AML causes the majority of orbital leukemic tumours [6]. AML involves the orbit in 30% of patients and is bilateral in one third those cases [2,6]. As it was in this case, a discreet leukemic mass called a myeloid sarcoma can form as the initial presentation of AML [6]. This extramedullary solid tumor has been referred to using less correct terms including a “chloroma” as it can occasionally have a greenish color clinically due to the presence of the pigment myeloperoxidase, and the misnomer, “granulocytic sarcoma” despite its lack of granulation tissue. Proptosis is the most common presenting sign of orbital myeloid sarcoma, while it can also present eyelid edema, epiphora, dacryoadenitis, extraocular muscle infiltration, motility disturbances or chemosis [7]. The lateral wall of the orbit is most commonly involved [6]. The prognosis of this type of tumors has improved in the last decades, with current survival rates between 60-80% [8]. Patients need an immediate work-up including orbital biopsy and co-management with a pediatric oncologist.
Conclusion
AML can present as an extramedullary tumor in childhood. Rapid diagnosis and systemic treatment, irrespective of systemic manifestations, is warranted to achieve the best possibility of long-term disease-free survival.
References
- Russo V, Scott I, Querques G, Stella A, Barone A, et al. (2008) Orbital and ocular manifestations of acute childhood leukemia: Clinical and statistical analysis of 180 patients. Eur J Ophthalmol 18: 619-623.
- Schwyzer R, Sherman GG, Cohn RJ, Poole JE, Willem P (1998) Granulocytic sarcoma in children with acute myeloblastic leukemia and t(8;21). Med Pediatr Oncol 31: 144-149.
- Byrd JC, Edenfield WJ, Shields DJ, Dawson NA (1995) Extramedullary myeloid cell tumors in acute nonlymphocytic leukemia: a clinical review. J Clin Oncol 13: 1800-18116.
- Templeton AC (1967) Tumors of the eye and adnexa in Africans of Uganda. Cancer 20: 1689-1698.
- Gürgey A, Yetgin S, Çetin M, Gümrük F, Tuncer A M, et al. (2004) Acute lymphoblastic leukemia in infants. Turk J Pediatr 46: 115-119.
- Bidar M, Wilson MW, Laquis SJ, Wilson TD, Fleming JC, et al. (2007) Clinical and Imaging Characteristics of Orbital Leukemic Tumors. Ophthalmic Plast Reconstr Surg 23: 87-93.
- Kiratli H, Balci KE, Himmetoglu Ç, Üner A (2009) Isolated extraocular muscle involvement as the ophthalmic manifestation of leukaemia. Clin Exp Ophthalmol 37: 609-613.
- Rubnitz JE, Lensing S, Zhou Y, Sandlund JT, Razzouk BI, et al. (2004) Death during induction therapy and first remission of acute leukemia in childhood. Cancer 101: 1677–1684.
Citation: Mvilongo C, Luciano AD, Plemel DJA, Afetane T, Epee E, et al. (2021) Bilateral Orbital Extension of Acute Myeloid Leukemia Masquerading as Burkitt Lymphoma: A Case Report. J Ophthalmic Clin Res 8: 084.
Copyright: © 2021 Caroline Mvilongo, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.

