
Health Coaching as a Pathway to Enhanced Psychological Well-Being: Results from an Observational Study
*Corresponding Author(s):
Romano RContract Professor At The University Of Parma, Italy
Email:rita.romano@unipr.it
Abstract
Background: Psychological well-being is increasingly recognized as a key determinant of overall health, influencing resilience, health behaviors, and long-term outcomes. Health Coaching (HC), a person-centered approach integrating cognitive-behavioral strategies and motivational techniques, has shown promise in enhancing psychological and behavioral outcomes. However, limited evidence exists on its direct impact on global well-being as measured by the Psychological General Well-Being Index (PGWBI).
Objective: This study aimed to evaluate the effectiveness of a structured health coaching program in improving perceived psychological well-being among participants enrolled in a Health Coaching educational pathway.
Methods: A quantitative quasi-experimental one-group pretest–posttest design was adopted. A total of 153 participants were assessed using the PGWBI before (January 2025) and after (November 2025) an 11-month structured health coaching program. The intervention included workshops, lifestyle education, and individual coaching sessions. Due to non-normal distribution of differences, nonparametric analyses were conducted, including the sign test for paired comparisons. The PGWBI total score was used as a global measure of psychological well-being.
Results: Participants showed a statistically significant improvement in psychological well-being, with PGWBI median scores increasing from 79 at baseline to 84 post-intervention (median change = +2). The direction of change was predominantly positive, with improvements significantly outweighing deteriorations. Subgroup analyses revealed no significant differences in outcomes across age, sex, educational level, or marital status. Internal consistency of the PGWBI was high (Cronbach’s α = 0.952).
Conclusions: Participation in a structured health coaching program was associated with a significant improvement in perceived psychological well-being. These findings support the potential role of health coaching as an effective intervention for enhancing subjective well-being in real-world educational settings. However, given the absence of a control group and the observational design, causal inferences remain limited. Future controlled and longitudinal studies are warranted to confirm these findings and to explore underlying mechanisms and long-term effects.
Keywords
Behavioral Change, Health Coaching, Psychological Well-Being, PGWBI (Psychological General Well-Being Index), Self-Regulation
Introduction
Over the last few decades, researchers have shown growing interest in the concept of perceived psychological well-being, that describes how people sense and evaluate their own emotional balance, sense of control, vitality, and overall satisfaction with life.
Within health psychology and public-health research, this perspective has become increasingly important since it stands as a basis for meaningful health aspects, including resilience to stressors, engagement in health-promoting behaviours, and long-term physical health goals.
Epidemiological and clinical studies have linked higher well-being scores to better recovery after health events, lower incidence of chronic disease, and in general reduced mortality risk. In addition, individuals who report higher levels of well-being tend to adopt healthier habits and experience more stable physical health over time, showing as psychological well-being not only acts as an indicator of mental health, but also as a meaningful predictor of overall quality of life.
To create a standardized way of assessing perceived psychological well-being, the Psychological General Well-Being Index (PGWBI) was developed as a concise self-report tool covering six core domains defined as anxiety, depressed mood, positive well-being, self-control, general health and vitality [1].
The original PGWBI consists of 22 items [1], although other subsequent shorter variants have been validated and widely used in community surveys, clinical trials and cross-cultural studies to monitor population health and to evaluate the efficacy of psychosocial interventions. The widespread and ongoing use of the PGWBI demonstrates its value as a practical and reliable tool for capturing overall psychological well-being, alongside established indicators of mental health and quality of life, in both research and clinical domains [2].
Alongside this, Health Coaching (HC) has emerged as a structured and evidence-based approach aimed at facilitating sustainable behavioural change through cognitive-behavioural principles, and personalized goal setting, basically focusing on strengthening self-regulation and intrinsic motivation.
In contrast to traditional medical models, which are primarily focused on disease treatment, Health Coaching involves a more holistic view of the human being, linking psychological, physical, and emotional aspects of well-being. Drawing on concepts from neuroscience, it recognizes how closely the brain, hormonal regulation, and immune function are connected in determining both behaviour and perceptions of the self.
This integrative perspective offers a clearer understanding of the ways in which stress responses, emotional regulation, and lifestyle patterns interact to shape overall health.
A growing body of empirical research supports the effectiveness of health coaching in enhancing different psychological and behavioural outcomes, including self-efficacy and self-esteem, even among individuals who initially report low self-perception [3,4]. Moreover, findings from clinical and community-based programs indicate consistent benefits in several health areas, such as weight management, metabolic regulation, and cardiovascular functioning, highlighting its relevance as a flexible, person-centred approach to sustaining long-term well-being [5,6].
Background
In recent years, the PGWBI has been increasingly adopted as an outcome measure to evaluate the psychological effects of Health Coaching interventions. Several studies have demonstrated that structured coaching programs lead to measurable improvements in perceived well-being within PGWBI domains.
As mentioned above, health coaching has been operationalized as a person-centred approach that combines motivational interviewing, cognitive-behavioural techniques and personalised goal-setting to promote self-regulation and sustainable behaviour change [7].
Randomized evidence indicate that HC produces small but consistent improvements in key behaviours and proximal psychological outcomes. In this context, An & Song reported a systematic review of 15 randomized controlled trials evaluating the impact of health coaching on psychological outcomes, showing statistically significant effects for physical activity and health responsibility [8]. Going into details, the authors synthesised data from controlled trials applying health coaching interventions to adults with cardiovascular risk factors. The included studies generally employed motivational interviewing and short educational sessions, delivered either face-to-face or by telephone. In addition, most interventions lasted between 3 and 12 months and key methodological features included use of peer coaches, structured goal-setting, and regular follow-up contacts.
The pooled results indicated small but statistically significant improvements in physical activity, dietary behaviours, health responsibility and stress management; however, no significant impact was observed on smoking behaviour. Among these studies, Vale et al., carried out a randomized trial involving 792 patients with coronary heart disease and reported a strong reduction cholesterol level, three times bigger than the control groups [9]. The intervention also improved adherence to lifestyle recommendations, supporting coaching as an effective secondary prevention strategy. In 2010, Wolever et al. developed a six-month health coaching program for 56 type-2 diabetic patients, showing improved self-care behaviours and psychosocial outcomes [7].
More recently, different studies have demonstrated that also mobile health coaching can improve physical activity levels and reduce average glucose concentrations over six months in case of diabetics [10], as well as lead to significant improvements in diet quality and consequent weight reduction, thus demonstrating that also digital coaching can effectively promote behavioural change in chronic disease management [11].
Finally, in their meta-analysis pooling 1842 participants across weight-loss interventions, Racey et al. found that not only health coaching was associated with a mean weight reduction of 2.4 kg (p < 0.01), but also with improvements in self-efficacy and life satisfaction, suggesting consistent psychological benefits beyond physical outcomes [12]. Although heterogeneous in design and outcomes, the consistency across domains supports the adoption of health coaching as a promising modality for supporting lifestyle change in at-risk adults.
However, to the best of our knowledge, just few reported works correlate health coaching with Psychological General Well-Being Index as tool for direct outcomes evaluation. For instance, very recently A. Pipio et al. [[13] used the 22-items PGWBI, among other tools, to assess the effects of the structured health coaching program Mastercap, showing both the efficacy of the program itself, and the effectiveness of the PGWBI as a monitoring tool for perceived psychological well-being.
Therefore, integrating the PGWBI into health-coaching programs could allow for a more accurate characterization of psychological improvements and could offer a coherent framework for examining how coaching-related processes translate into behavioural adjustments and subsequent health benefits.
Aim
Building on existing evidence, the present study aims to evaluate the effectiveness of a structured health-coaching program in improving perceived psychological well-being, as measured by the Psychological General Well-Being Index (PGWBI). By systematically evaluating pre – post changes across the instrument core domains, the study seeks to clarify whether individualized coaching-based interventions can contribute to measurable improvements in global psychological wellness, thereby addressing the current gap in the literature and assisting the design of future integrative health-coaching strategies.
Research Question
Can participation in a structured health coaching program reduce perceived psychophysical stress among students enrolled in a Health Coaching educational pathway?
Hypotheses
H1. Participation in the health coaching program will be associated with a significant reduction in perceived psychophysical stress from baseline to post-intervention.
Methods
Study Design
This study adopted a quantitative quasi-experimental one-group pretest-posttest design without a control group. The intervention was delivered over an 11-month period within a naturalistic educational context, corresponding to the regular training activities of the Health Coaching Program. This design was selected to assess within-subject changes over time in perceived psychophysical stress and sleep quality following participation in the program.
Participants
Participants were recruited through convenience sampling from students enrolled in the first and second year of the Health Coaching Program at the Health Coaching Academy. All students attending the program during the data collection period were considered eligible for inclusion. Inclusion criteria were enrollment in the program at the time of the study and provision of informed consent to participate. No exclusion criteria were applied, as the study aimed to capture the experience of the entire accessible cohort and to reflect the ecological characteristics of the educational setting.
Instruments
In the present study, perceived psychological well-being was assessed using the Italian version of the Psychological General Well-Being Index (PGWBI), a 22-item self-report instrument referring to the previous four weeks and originally conceptualized into six domains: anxiety, depressed mood, positive well-being, self-control, general health, and vitality [1]. Items are rated on six-point Likert-type scales and, according to the standard scoring procedure, negatively worded items require reverse coding. The sum of item scores yields a global index ranging from 0 to 110, with higher scores indicating better subjective psychological well-being [1]. Although the PGWBI has historically been described in terms of six subdimensions, the present study used only the total score and not factor-specific scores. This choice was based on psychometric evidence suggesting that the robustness of the original factorial structure is not sufficiently stable across validation studies. Previous investigations have shown that the six-factor solution is not consistently replicated and that alternative latent structures may emerge in different samples. In addition, Rasch analysis has suggested that, after accounting for local item dependencies, the PGWBI is more appropriately interpreted as reflecting a dominant general dimension of psychological well-being rather than a set of clearly independent subscales. Therefore, in line with the available psychometric literature, the PGWBI was analyzed in this study as a continuous global measure of perceived psychological well-being, as this approach appears methodologically more robust and conceptually more defensible than the use of separate factor scores.
In our study, internal consistency assessed using the overall Cronbach’s alpha was α = .952), in line with the values reported in an Italian study (α = .94) [1].
Procedure
The study was conducted in four sequential phases:
- Recruitment and informed consent: Students were informed about the study objectives and procedures during scheduled academic activities. Participation was voluntary, and informed consent was obtained along with privacy documentation.
- Baseline assessment (January 2025): Participants completed PGWBI questionaire.
- Intervention (February–November 2025): The health coaching program included:
- In-person workshops on coaching techniques and neuro-linguistic programming (NLP);
- Educational modules promoting healthy lifestyle behaviors (e.g., mindful nutrition, regular physical activity);
- Five one-to-one health coaching sessions delivered by certified professionals registered with the national professional association.
- Follow-up assessment (November 2025): The same questionnaires PGWBI were re-administered to assess changes in perceived psychological well-being.
Data Analysis
Descriptive statistics (means, standard deviations, frequencies) will be computed for all variables. The differences (D = post − pre) were not normally distributed for any of the outcomes, as indicated by significant Shapiro–Wilk tests (p < .05), with n = 152 valid cases. This finding supports the use of nonparametric methods and, in the presence of marked asymmetry and/or an accumulation of zero differences, makes the use of the sign test methodologically appropriate, as it relies only on the direction of change and excludes ties
Results
Descriptive analyses
The analyzed sample comprised 153 participants.
Regarding the “course” variable, 39.9% were in category 8 (n=61), 39.9% in category 9 (n=61), and 20.3% in category adv (n=31).
The sample was predominantly female (67.3%, n=103), while males accounted for 32.7% (n=50).
Educational attainment was mainly upper secondary school (45.8%, n=70), followed by university degree (27.5%, n=42) and postgraduate education (17.0%, n=26), with smaller proportions reporting lower secondary school (9.2%, n=14) and no formal qualification (0.7%, n=1).
For marital/social status, the most represented categories were married (32.0%, n=49) and single (31.4%, n=48), followed by cohabiting (17.6%, n=27), separated (9.2%, n=14), divorced (9.2%, n=14), and widowed (0.7%, n=1); 83.0% (n=127) reported living with others, and 17.0% (n=26) living alone.
Employment status indicated that most participants were in paid employment (85.6%, n=131), with smaller proportions of students (8.5%, n=13), unemployed (1.3%, n=2), and other employment conditions (4.6%, n=7).
With respect to self-reported illnesses, 56.2% (n=86) reported no illness, 34.0% (n=52) reported minor conditions, and 9.8% (n=15) reported conditions of moderate/severe seriousness; mean age was 43.0 years (SD 14.4).
[Tables 1&2] summarize the pre- and post-intervention outcomes, reported as median (IQR) due to the skewed distribution, together with the median change (Δ= POST–PRE).
Pre–post change was then evaluated using the sign of paired differences with the sign test (two-tailed exact binomial), reporting n+, n−, n0, the exact p-value, and the proportion of positive changes with 95% CI.
 Table 1: Pre- and post-intervention outcomes for PGWBI, reported as median (IQR), with the median paired change (Δ= POST−PRE) and its IQR.
Table 1: Pre- and post-intervention outcomes for PGWBI, reported as median (IQR), with the median paired change (Δ= POST−PRE) and its IQR.
 Table 2: Wilcoxon signed-rank test for paired PRE–POST comparisons of PGWBI, reporting the number of discordant pairs (POST>PRE; POST< PRE), ties, effective sample size (n_eff), standardized Z, and exact two-sided p values. The effect-size estimate p = n+/n_eff summarizes the probability of a positive change (probability of superiority) with its confidence interval.
Table 2: Wilcoxon signed-rank test for paired PRE–POST comparisons of PGWBI, reporting the number of discordant pairs (POST>PRE; POST< PRE), ties, effective sample size (n_eff), standardized Z, and exact two-sided p values. The effect-size estimate p = n+/n_eff summarizes the probability of a positive change (probability of superiority) with its confidence interval.
The following tables report subgroup analyses of the change scores (Δ POST−PRE) for PGWBI across age groups, sex, educational attainment, and marital/social status, presenting descriptive statistics (median, IQR) and between-group comparisons using nonparametric tests (Kruskal–Wallis; Mann–Whitney U), together with the corresponding effect-size measures (ε² and r) [Tables 3-6].
 Table 3: Change scores (Δ POST–PRE) for sleep perception and stress perception across age classes, reported as median (IQR) and compared using the Kruskal–Wallis test
Table 3: Change scores (Δ POST–PRE) for sleep perception and stress perception across age classes, reported as median (IQR) and compared using the Kruskal–Wallis test
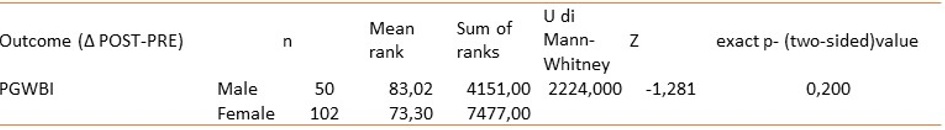 Table 4: Change scores (Δ POST–PRE) for PGWBI perception by sex and compared using the Mann–Whitney U test (U, Z, exact two-sided p).
Table 4: Change scores (Δ POST–PRE) for PGWBI perception by sex and compared using the Mann–Whitney U test (U, Z, exact two-sided p).
 Table 5: Change scores (Δ POST–PRE) for PGWBI perception across educational attainment levels, reported Mean /Sum rank and compared using the Kruskal–Wallis test
Table 5: Change scores (Δ POST–PRE) for PGWBI perception across educational attainment levels, reported Mean /Sum rank and compared using the Kruskal–Wallis test
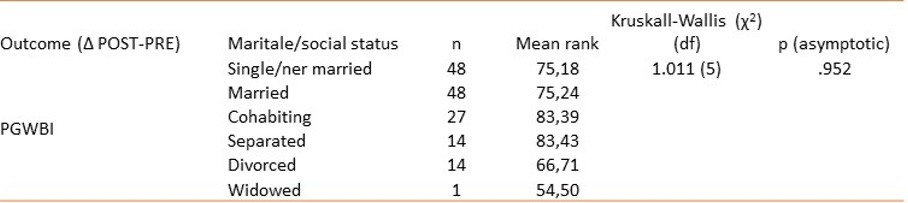 Table 6: Change scores (Δ POST–PRE) for PGWBI perception across marital/social status categories, reported mean runk and compared using the Kruskal–Wallis test
Table 6: Change scores (Δ POST–PRE) for PGWBI perception across marital/social status categories, reported mean runk and compared using the Kruskal–Wallis test
Discussion
The present study shows a statistically significant improvement in perceived psychological well-being after participating in a structured health coaching program. The PGWBI total score increased from a median of 79 at baseline to 84 post-intervention, with a median variation of 2 points. Paired analysis also showed that improvements outweighed deteriorations, indicating an overall favorable direction of change. Taken together, these findings support the study hypothesis, confirming that participation in the health coaching program was associated with an increase in subjective psychological well-being.
From an interpretive perspective, these findings are consistent with the theoretical rationale of health coaching, acting on self-regulation, self-awareness, goal setting, and personal activation. These processes may result in greater perceived control, improved emotional stability, and a more favorable assessment of general well-being. In this respect, the results are in line with previous literature describing beneficial effects of coaching on proximal psychological outcomes and health behaviors, despite heterogeneity in settings, intervention models, and outcome measures.
A further strength concerns the outcome measure. In the present sample, the PGWBI showed high internal consistency. In addition, the choice of using the total score rather than factor-specific scores appears methodologically appropriate on a psychometric literature basis, which does not consistently support the stability of the original factorial structure. This supports a more defensible interpretation of the PGWBI as a global indicator of perceived psychological well-being.
Subgroup analyses show no statistically significant differences in PGWBI variation according to age, sex, educational attainment, or social status. This may suggest that the observed association was not confined to a specific sociodemographic profile. However, this interpretation should remain cautious, as some categories were numerically small and the study was not designed or powered for stratified comparisons. These findings should therefore be regarded as exploratory.
The study has relevant limitations. First, the absence of a control group precludes strong causal inference and does not allow to exclude alternative explanations, including maturation, regression to the mean, participant expectancy, or the influence of external events during the observation period. Moreover, sampling within a specific educational pathway could limit the generalizability of the findings. In addition, reliance on a self-report outcome introduces the possibility of response bias. Finally, the multicomponent nature of the program does not allow to identify the specific intervention elements which are primarily responsible for the observed change, and also to draw any conclusions on the durability of the effect in the absence of dedicated follow-up.
Despite these limitations, the study also shows some strong points. First of all, it was conducted in a real-world setting, including the full accessible cohort, and furthermore an analytical strategy consistent with the distributional properties of the data was adopted. In particular, the use of nonparametric methods and the sign test was methodologically appropriate given the non-normal distribution of pre-post differences and the presence of ties. Within these boundaries, the findings may be interpreted as a coherent preliminary signal of the potential effectiveness of health coaching for improving perceived psychological well-being.
Conclusion
Participation in the structured health coaching program was associated with a significant improvement in perceived psychological well-being as measured by the PGWBI total score. The overall direction of change was favorable, and no significant differences were detected across the main subgroup analyses.
Overall, the findings support the potential role of health coaching as an educational and personal development intervention aimed at promoting subjective psychological well-being. However, interpretation should remain cautious given the uncontrolled design and the naturalistic nature of the study. Future studies using controlled designs, longitudinal follow-up, and process evaluation are needed to confirm the observed association, to clarify its mechanisms, and to assess its long-term stability.
Acknowledgement
We would like to thank all the Health Coaches who contributed to the realization of the project, the organizational secretariat of the health coaching Academy (Lucia Pieroni and Pamela Corbara) and all the students who took part in the study contributing to the scientific research.
References
- Grossi E, Compare A (2024) Psychological general well-being index (PGWB). InEncyclopedia of quality of life and well-being research. Cham: Springer International Publishing 5541-5546.
- Wang IY, Cheung RY (2024) Psychological General Well-Being Index (PGWBI). InHandbook of Assessment in Mindfulness Research. Cham: Springer International Publishing 1-10.
- An S, Song R (2020) Effects of health coaching on behavioral modification among adults with cardiovascular risk factors: Systematic review and meta-analysis. Patient Education and Counseling 103: 2029-2038.
- Kim Y, Lee S (2023) A systematic review and meta-analysis of the effectiveness of non-face-to-face coaching. Sustainability 15: 9727.
- Almulhim AN, Hartley H, Norman P, Caton SJ, Dogru OC, et al. (2023) Behavioural change techniques in health coaching-based interventions for type 2 diabetes: a systematic review and meta-analysis. BMC Public Health 23: 95.
- Meng F, Jiang Y, Yu P, Song Y, Zhou L, et al. (2023) Effect of health coaching on blood pressure control and behavioral modification among patients with hypertension: A systematic review and meta-analysis of randomized controlled trials. International journal of nursing studies 138: 104406.
- Wolever RQ, Dreusicke M, Fikkan J, Hawkins TV, Yeung S, et al. (2010) Integrative health coaching for patients with type 2 dia The Diabetes Educator 36: 629-39.
- An S, Song R (2020) Effects of health coaching on behavioral modification among adults with cardiovascular risk factors: Systematic review and meta-analysis. Patient Education and Counseling 103: 2029-38.
- Vale MJ, Jelinek MV, Best JD, Dart AM, Grigg LE, et (2003) Coaching patients On Achieving Cardiovascular Health (COACH): a multicenter randomized trial in patients with coronary heart disease. Archives of Internal Medicine 163: 2775-83.
- Wayne N, Perez DF, Kaplan DM, Ritvo P (2015) Health coaching reduces HbA1c in type 2 diabetic patients from a lower-socioeconomic status community: a randomized controlled trial. Journal of medical Internet research 17: e224.
- Willard-Grace R, Chen EH, Hessler D, DeVore D, Prado C, et al. (2015) Health coaching by medical assistants to improve control of diabetes, hypertension, and hyperlipidemia in low-income patients: a randomized controlled trial. The Annals of Family Medicine 13: 130-138.
- Racey M, Jovkovic M, Alliston P, Ali MU, Sherifali D (2022) Diabetes health coach in individuals with type 2 diabetes: a systematic review and meta analysis of quadruple aim outcomes. Frontiers in endocrinology 13: 1069401.
- Pipio A, Romano R, Sollami A, La Rosa G, Malagò G, et al. (2025) Health Coaching: A Model for Enhancing Quality of Life. J Psychiatry Depression Anxiety 11: 056.
Citation: Pipio A, Romano R, Sollami A, Marino A, Malagò G, et al. (2026) Health Coaching as a Pathway to Enhanced Psychological Well-Being: Results from an Observational Study. HSOA J Psychiatry Depress Anxiety 12: 067.
Copyright: © 2026 Pipio A, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.

