
Impact assessment of structured health coaching intervention on perceived stress and sleep quality
*Corresponding Author(s):
Romano RContract Professor At The University Of Parma, Italy
Email:rita.romano@unipr.it
Abstract
Background: Perceived stress and sleep quality are key determinants of physical and psychological well-being, yet both are often impaired in populations exposed to demanding environments. Health coaching—an evidence-based, person-centred behavioural intervention—has shown promise in supporting stress reduction and lifestyle improvement, but its effects on perceived stress and subjective sleep quality remain insufficiently characterized.
Objective: This study aimed to evaluate the impact of an 11-month structured health coaching program on perceived stress, assessed through the Perceived Stress Scale (PSS-10), and sleep quality, measured using the Pittsburgh Sleep Quality Index (PSQI), among adult learners enrolled in a health coaching training program.
Methods: A quantitative quasi-experimental pre–post design without a control group was implemented. A total of 153 participants completed baseline (January 2025) and follow-up (November 2025) assessments. The intervention comprised in-person workshops, educational lifestyle modules, and five individual coaching sessions delivered by certified health coaches. Due to non-normality of pre–post differences, changes were analysed using nonparametric paired tests (sign test and Wilcoxon signed-rank test), complemented with effect size estimates.
Results: Significant improvements were observed for both outcomes. Participants showed a statistically significant reduction in perceived stress and an improvement in sleep quality (p < 0.001 for both), with median pre–post changes indicating favourable shifts in self-reported well-being. Probability-of-superiority indices supported the robustness of these effects. Subgroup analyses (age, sex, education, marital status) revealed no significant between-group differences, suggesting consistent benefits across demographic profiles.
Conclusions: Participation in a structured health coaching program was associated with meaningful reductions in perceived stress and improved sleep quality. These findings support the potential of health coaching as a scalable, non-pharmacological approach to promoting psychological well-being. Future controlled studies with objective sleep metrics and longer follow-up are warranted to strengthen causal inference and assess long-term sustainability.
Introduction
Perceived stress and sleep quality are closely interrelated concepts that play a central role in physiological well-being. Elevated stress levels have been consistently associated with impaired sleep quality, dysregulation of the hypothalamic – pituitary – adrenal (HPA) axis, and an increased risk of anxiety, depression, and cardiometabolic disorders [1,2]. Sleep disturbances, in turn, intensify emotional reactivity and reduce the individual ability to effectively manage daily stressors, creating a bidirectional relationship that perpetuates maladaptive health outcomes [3,4].
In this context, perceived stress represents a critical psychological construct associated with adverse health outcomes including cardiovascular disease, immune dysregulation, depression, and burnout [1,5]. The Perceived Stress Scale (PSS), particularly its 10- and 14-item versions (PSS-10, PSS-14), remains among the most widely validated self-report instruments for quantifying subjective stress appraisal [6,7]. Evidence from both clinical and non-clinical populations has demonstrated that elevated PSS scores are associated with poorer physical and mental health, reduced work performance, and lower quality of life [7,8].
On the other hand, sleep quality can be assessed by means of the Pittsburgh Sleep Quality Index (PSQI), i.e., a validated self-report questionnaire that evaluates subjective sleep quality and disturbances over time [9]. The PSQI consists of 9 fundamental items aggregated into seven components, which are subjective sleep quality, sleep latency, sleep duration, habitual sleep efficiency, sleep disturbances, use of sleeping medication, and daytime dysfunction, with higher scores indicating poorer sleep quality. This instrument has demonstrated strong internal consistency, test–retest reliability, and construct validity across both clinical and non-clinical populations, and it is widely regarded as a gold standard for assessing perceived sleep quality in behavioural and health research [9-11].
Within this framework, health coaching has emerged as a structured, client-centred behavioural intervention designed to promote self-regulation, resilience, and sustainable lifestyle change through motivational interviewing, goal-setting, and psychosocial support [12]. Consequently, integrating health coaching within stress management and sleep improvement programs may represent a promising approach to support long-term well-being and prevent stress-induced health deterioration.
Background
Although coaching was originally applied within executive and athletic contexts, recent developments in public health and behavioural medicine have extended its application to chronic disease management, lifestyle behaviour change, and stress reduction [13,14].
Several randomized controlled trials (RCTs) and quasi-experimental studies have investigated the efficacy of health coaching on perceived stress as quantified by the PSS-10 and PSS-14. For example, a digital Mindfulness-Based Stress Reduction (MBSR) program incorporating coach consultations demonstrated a significant PSS-10 reduction of 4.86 points in 12 weeks, with sustained effects after six months [15]. In occupational contexts, Ene et al. reported that a rational-emotive occupational health coaching intervention significantly decreased PSS scores among academic staff, providing empirical support for the utility of cognitive-behavioural coaching frameworks for mitigating workplace stress [16]. Similarly, Ziaka et al. carried out an 8-week stress management and health coaching intervention among office workers, which also resulted in a significant decrease in PSS-14 (p = 0.043), maintained over time [17]. A more recent study (Rose G.L. et al., 2025) demonstrated that in a 12-week employee health and wellness coaching intervention, combining individual and group sessions, participants exhibited significant reductions in perceived stress as measured by the PSS-10, with improvements maintained at sixth and twelfth week follow-ups. Moreover, the authors showed that additional text-message support did not lead to further reductions, indicating that the active coaching sessions were the primary driver of stress improvement [18].
In their systematic review, Wolever et al. [12] examined how the intensity of health and wellness coaching interventions can be related to effectiveness. The reported results show that programs offering a higher dose of coaching, in terms of number of sessions or time duration, generally led to greater improvements in health behaviours and outcomes. Nevertheless, the authors noted that the optimal dose is context-dependent, varying according to the intervention setting, the targeted behaviour, and the characteristics of the population. They also highlighted the need for further research to identify the most effective dosing strategies for different types of coaching and contexts [12].
Despite this growing body of empirical data, heterogeneity in intervention design, coaching modality, and stress measurement has limited analytic clarity regarding the strength and consistency of this relationship. Furthermore, the mechanistic pathways by which coaching influences perceived stress and sleep quality via cognitive reappraisal, emotional self-regulation, or behaviour change, remain incompletely characterized to the best of our knowledge [19].
Aim
On the basis of literature analysis, the present study aims to address the research gap by systematically evaluating the impact of structured health coaching interventions on perceived stress, as measured by validated PSS instrument, and on sleep quality, as assessed by the PSQ, with the ultimate goal of clarifying the therapeutic utility of health coaching, thus providing insights for optimizing future interventions.
Research Question
Can a structured health coaching program reduce perceived stress and improve sleep quality?
Hypotheses
H1: Participation in the health coaching program will result in a significant reduction in psychophysical stress.
H2: Participation in the health coaching program will result in a significant improvement in sleep quality.
Methods
Study Design
This study employed a quantitative quasi-experimental pre–post design without a control group.
The intervention lasted 11 months and was implemented in a naturalistic educational setting.
Participants
Participants were recruited through convenience sampling from students enrolled in the first and second year of the Health Coaching Program at the Health Coaching Academy. Eligibility criteria included enrolment in the program at the time of data collection and provision of informed consent.
Exclusion criteria were not applied, as the study aimed to capture the entire cohort’s experience.
Instruments
Perceived Stress: Measured using the Perceived Stress Scale (PSS-10; Cohen, 1997), Italian version (Messineo e Tosto, 2024) [20]. The instrument consists of 10 items rated on a 5-point Likert scale (0 = never; 4 = very often), The PSS-10 score was calculated by reverse-coding items 4, 5, 7, and 8 and then summing all 10 items (range 0 - 40), with higher scores indicating greater perceived stress (Messineo & Tosto, 2024).
In our study, internal consistency assessed using the overall Cronbach’s alpha was α = 0.88 (α = 0.78 and α = 0.88 for the negative and positive subscales, respectively), in line with the values reported in the Italian validation study (α = 0.75; α = 0.87; α = 0.77; [20]).
Sleep Quality: Sleep was assessed using the Pittsburgh Sleep Quality Index (PSQI) of Buysse and colleagues (1989), in the Italian version by Curcio and colleagues (2013) [21], a self-rated questionnaire referring to the previous month. The PSQI comprises 19 items from which seven components are derived (subjective sleep quality, sleep latency, sleep duration, habitual sleep efficiency, sleep disturbances, use of sleeping medication, and daytime dysfunction), yielding component scores (0-3) and a global score obtained by summing these components (range 0–21), with higher scores indicating poorer sleep quality. In our study, the instrument’s reliability, assessed using Cronbach’s alpha, was α = 0.81, comparable to that reported in the Italian validation study (α = 0.85; [21]).
Procedure
The study was conducted in four sequential phases:
- Recruitment and informed consent: Students were informed about the study objectives and procedures during scheduled academic activities. Participation was voluntary, and informed consent was obtained along with privacy documentation.
- Baseline assessment (January 2025): Participants completed the PSS-10 and PSQI questionnaires.
- Intervention (February–November 2025): The health coaching program included:
- In-person workshops on coaching techniques and neuro-linguistic programming (NLP);
- Educational modules promoting healthy lifestyle behaviors (e.g., mindful nutrition, regular physical activity);
- Five one-to-one health coaching sessions delivered by certified professionals registered with the national professional association.
- Follow-up assessment (November 2025): The same questionnaires (PSS-10 and PSQI) were re-administered to assess changes in perceived stress and sleep quality.
Data Analysis
Descriptive statistics (means, standard deviations, frequencies) will be computed for all variables.
The paired differences Δ = post−pre for perceived stress and for the sleep-quality indicator are not normally distributed in the normality tests run in SPSS, which provides a methodological justification for using nonparametric tests for the pre-post comparison.
Specifically, for Dstress the Shapiro–Wilk test is W = 0.976 with p < 0.05, and for Dsleep the Shapiro–Wilk test is W = 0.917 with p < 0.001, indicating a statistically significant deviation from normality (α = 0.05).
Consistently, the paired comparisons show a pattern of differences compatible with asymmetric distributions and many ties (zero differences), a condition under which a nonparametric approach based on the direction of change (sign test) is appropriate.
Results
Descriptive analyses
The analysed sample comprised 153 participants.
Regarding the “course” variable, 39.9 % were in category 8 (n = 61), 39.9 % in category 9 (n = 61), and 20.3 % in category adv (n = 31).
The sample was predominantly female (67.3 %, n = 103), while males accounted for 32.7 % (n = 50).
Educational attainment was mainly upper secondary school (45.8 %, n = 70), followed by university degree (27.5 %, n = 42) and postgraduate education (17.0 %, n = 26), with smaller proportions reporting lower secondary school (9.2 %, n = 14) and no formal qualification (0.7 %, n = 1).
For marital/social status, the most represented categories were married (32.0 %, n = 49) and single (31.4 %, n = 48), followed by cohabiting (17.6 %, n = 27), separated (9.2 %, n = 14), divorced (9.2 %, n = 14), and widowed (0.7 %, n = 1); 83.0 % (n = 127) reported living with others, and 17.0 % (n = 26) living alone.
Employment status indicated that most participants were in paid employment (85.6 %, n = 131), with smaller proportions of students (8.5 %, n = 13), unemployed (1.3 %, n = 2), and other employment conditions (4.6 %, n = 7).
With respect to self-reported illnesses, 56.2 % (n = 86) reported no illness, 34.0 % (n = 52) reported minor conditions, and 9.8 % (n = 15) reported conditions of moderate/severe seriousness; mean age was 43.0 years (SD 14.4).
[Tables 1&2] summarize the pre- and post-intervention outcomes, reported as median (IQR) due to the skewed distribution, together with the median change (Δ = POST−PRE).
Pre–post change was then evaluated using the sign of paired differences with the sign test (two-tailed exact binomial), reporting n+, n−, n0, the exact p-value, and the proportion of positive changes with 95% CI.
 Table 1: Pre- and post-intervention outcomes for sleep perception and stress, reported as median (IQR), with the median paired change (Δ= POST−PRE) and its IQR.
Table 1: Pre- and post-intervention outcomes for sleep perception and stress, reported as median (IQR), with the median paired change (Δ= POST−PRE) and its IQR.
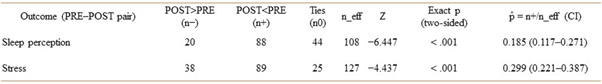
Table 2: Wilcoxon signed-rank test for paired PRE–POST comparisons of sleep perception and stress, reporting the number of discordant pairs (POST>PRE; POST<PRE), ties, effective sample size (n_eff), standardized Z, and exact two-sided p values. The effect-size estimate p = n+/n_eff summarizes the probability of a positive change (probability of superiority) with its confidence interval.
The following [Table 3-6] report subgroup analyses of the change scores (Δ POST−PRE) for sleep perception and stress across age groups, sex, educational attainment, and marital/social status, presenting descriptive statistics (median, IQR) and between-group comparisons using nonparametric tests (Kruskal–Wallis; Mann–Whitney U), together with the corresponding effect-size measures (ε2 and r).
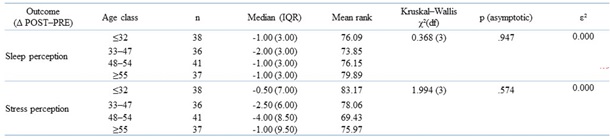
Table 3: Change scores (Δ POST–PRE) for sleep perception and stress perception across age classes, reported as median (IQR) and compared using the Kruskal–Wallis test with effect size ε2.
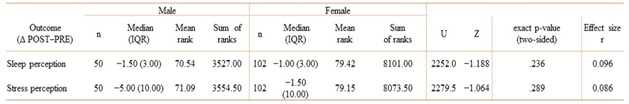
Table 4: Change scores (Δ POST–PRE) for sleep perception and stress perception by sex, reported as median (IQR) and compared using the Mann–Whitney U test (U, Z, exact two-sided p) with effect size r.
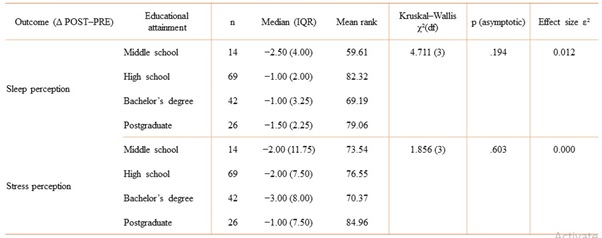
Table 5: Change scores (Δ POST–PRE) for sleep perception and stress perception across educational attainment levels, reported as median (IQR) and compared using the Kruskal–Wallis test with effect size ε2.
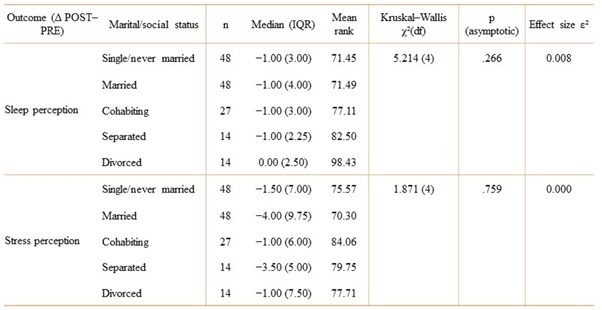 Table 6: Change scores (Δ POST–PRE) for sleep perception and stress perception across marital/social status categories, reported as median (IQR) and compared using the Kruskal–Wallis test with effect size ε².
Table 6: Change scores (Δ POST–PRE) for sleep perception and stress perception across marital/social status categories, reported as median (IQR) and compared using the Kruskal–Wallis test with effect size ε².
Discussion
The results of this study consistently support both proposed hypotheses, indicating that participation in a health coaching program is associated with (H1) a significant reduction in psycho-physical stress and (H2) an improvement in sleep quality.
From a descriptive standpoint, pre-post median values show a decrease in both perceived sleep, with a negative median change, and stress, with a more pronounced median reduction, yielding an overall pattern consistent with a beneficial effect of the intervention on both self-reported outcomes. Inferential analysis of paired observations reveals statistically significant differences for both outcomes (p < 0.001), suggesting that the observed changes are unlikely to reflect random variation within the sample under study (see Tables 1 and 2).
From an interpretative perspective, these findings are consistent with the theoretical mechanisms commonly attributed to health and wellness coaching, including person-centred goal setting, the promotion of self-monitoring and personal accountability, and the use of strategies grounded in behaviour change theory [22]. Within this framework, coaching may act as a bridge between intention and behaviour, narrowing the gap between general recommendations (e.g., sleep hygiene, stressor management) and day-to-day adherence, with potential perceived benefits for rest and psychological distress [22]. Moreover, reductions in stress and improvements in daily routines are outcomes frequently reported in interventions combining coaching components with stress management techniques, including workplace-based settings, with evidence of effectiveness on perceived stress and sleep related domains [23].
A relevant feature of the dataset is the presence of a non-negligible proportion of pre-post ties, i.e., no change observation, suggesting a non-uniform effect across participants. This aspect is clinically informative, as it points to the possible coexistence of responders and non-responders and highlights the importance of incorporating in future studies moderation analyses, such as baseline severity, exposure to stressors, adherence to the program, and process evaluations, e.g., effective dose, intervention fidelity, and quality of the coaching relationship [24].
From a more comprehensive reporting perspective, the use of effect measures that are interpretable for ordinal or non-normally distributed data (e.g., probability of superiority, common language effect size) helps to characterise both the direction and magnitude of change beyond statistical significance alone [25].
Exploratory analyses across sociodemographic subgroups (sex, age groups, educational level, social status) did not reveal statistically significant differences in Δ (post-pre) changes, with small or negligible effect sizes.
Despite the inherent limitations of subgroup analyses, this finding suggests that the favourable association between coaching and outcomes may not be confined to a single demographic category, but rather distributed relatively broadly. Nevertheless, it should be noted that a lack of statistical significance does not imply equivalence between groups and may reflect limited statistical power or high variability (see Tables 3-6).
From a methodological standpoint, reporting effect size indices for non-parametric tests (e.g., ε2 for Kruskal-Wallis, r for Mann-Whitney) is recommended to quantify the practical relevance of findings, particularly when results are “non-significant” and when the aim is to avoid dichotomous interpretations based just on p-values [26].
Limitations
These results should be interpreted in light of some limitations affecting their inferential strength. Firstly, a pre-post design without a control group reduces the ability to causally attribute observed changes to health coaching, since regression to the mean, seasonal changes, concurrent events, and participants expectations may all have influenced the observed outcomes [24]. Moreover, the use of self-reported measures exposes the findings to social desirability and response biases, which are quite expected in interventions that emphasise relational and motivational support [22]. Finally, statistical significance does not automatically imply a substantial clinical impact.
Accordingly, future researches would benefit from pre-specifying minimal clinically important difference thresholds, integrating objective measures where possible (e.g., digital or actigraphy-based sleep indices), and evaluating the durability of effects over follow-up periods [24].
Conclusions
In terms of implications, the data support the inclusion of health coaching as a non-pharmacological, person-centred intervention that may be beneficial for subjectively reported outcomes of high relevance to health and daily functioning, such as stress and sleep [22]. Given that the literature suggests coaching may also facilitate the maintenance of changes and gains over time, the next priority is to design controlled and pragmatic studies evaluating comparative effectiveness, organizational sustainability, and cost–benefit considerations, while incorporating measures of adherence and implementation [24].
In summary, the evidence from this sample indicates a statistically significant improvement in stress and perceived sleep following health coaching, with no substantial differences observed across demographic subgroups, and underscores the need for strengthened methodological approaches in future evaluations to consolidate the clinical and organizational interpretation of the results.
Acknowledgement
We would like to thank all the Health Coaches who contributed to the realization of the project, the organizational secretariat of the health coaching Academy (Lucia Pieroni and Pamela Corbara) and all the students who took part in the study contributing to the scientific research.
References
- Cohen S, Janicki-Deverts D, Miller GE (2007) Psychological stress and disease. JAMA 298: 1685-1687.
- Schneiderman N, Ironson G, Siegel SD (2005) Stress and health: psychological, behavioral, and biological determinants. Annual Review of Clinical Psychology 1: 607-628.
- Akerstedt T (2006) Psychosocial stress and impaired sleep. Scandinavian Journal of Work, Environment & Health 32: 493-501.
- Kim EJ, Dimsdale JE (2007) The effect of psychosocial stress on sleep: a review of
polysomnographic evidence. Behavioral Sleep Medicine 5: 256-278. - Schneiderman N, Ironson G, Siegel SD (2005) Stress and health: psychological, behavioral, and biological determinants. Annu Rev Clin Psychol 1: 607-628.
- Cohen S, Kamarck T, Mermelstein R (1983) A global measure of perceived stress. J Health Soc Behav 24: 385-396.
- Lee EH (2012) Review of the psychometric evidence of the Perceived Stress Scale. J Psychosom Res 69: 307-314.
- Kocalevent RD, Levenstein S, Fliege H, Schmid G, Hinz A, et al. (2007) Contribution to the construct validity of the Perceived Stress Questionnaire from a population-based survey. J Psychosom Res 63: 71-81.
- Buysse DJ, Reynolds III CF, Monk TH, Berman SR, Kupfer DJ (1989) The Pittsburgh Sleep Quality Index (PSQI): A new instrument for psychiatric research and
Psychiatry Research 28: 193-213. - Backhaus J, Junghanns K, Broocks A, Riemann D, Hohagen F (2002) Test–retest reliability and validity of the Pittsburgh Sleep Quality Index in primary insomnia. Journal of Psychosomatic Research 53: 737-740.
- Mollayeva T, Thurairajah P, Burton K, Mollayeva S, Shapiro CM, et al. (2016) The Pittsburgh Sleep Quality Index as a screening tool for sleep dysfunction in clinical and
non-clinical samples: A systematic review and meta-analysis. Sleep Medicine Reviews 25: 52-73. - Wolever RQ (2016) Coaching in healthcare: a systematic review. Med Care 54: 707-715.
- Wolever RQ, Moore MA, Jordan M (2017) Coaching and health. In: Bachkirova T, et al. The SAGE Handbook of Coaching. SAGE 521-543.
- Palmer S, Tubbs I, Whybrow A (2003) Health coaching: is it effective? Int J Evid Based Coach Mentor 1: 9-17
- Venkatesan A, Krymis H, Scharff J, Waber A (2021) Changes in Perceived Stress Following a 10-Week Digital Mindfulness-Based Stress Reduction Program: Retrospective Study. JMIR Form Res 5: e25078.
- Ene CU, Ugwuanyi CS, Ejimonye JC, Ani MI, Eneogu ND, Ikeh FE, Eya NM, Oguguo BC, Ibenegbu QO, Odionye N, Monday S (2021) Effects of rational emotive occupational
health coaching on work stress among academic staff of science and social science education in Nigerian universities: A randomised trial evaluation. Medicine 100: e26963. - Ziaka D, Tigani X, Kanaka-Gantenbein C, Alexopoulos EC (2025) A Stress Management and Health Coaching Intervention to Empower Office Employees to Better Control Daily Stressors and Adopt Healthy Routines. Int J Environ Res Public Health 22: 548.
- Rose GL, Smith AM, Mossburg J, Westervelt K (2025) Impact of an Employee Health and Wellness Coaching Program on Self-Reported Stress, Physical Health, and Mental Health in Hospital and University Employees. Glob Adv Integr Med Health 14: 27536130251363933.
- Grant AM, Cavanagh MJ (2007) Evidence-based coaching: flourishing or languishing? Australian Psychologist 42: 239-254.
- Messineo L, Tosto C (2024) Evaluation of the psychometric properties of the Italian version of the 10-item perceived stress scale in a sample of teachers. Frontiers in Psychology 14: 1330789.
- Curcio G, Tempesta D, Scarlata S, Marzano C, Moroni F, et al. (2013) Validity of the Italian version of the Pittsburgh Sleep Quality Index (PSQI). Neurological Sciences 34: 511-519.
- Wolever RQ, Simmons LA, Sforzo GA, Dill D, Kaye M, et al. (2013) A systematic review of the literature on health and wellness coaching: Defining a key behavioral intervention in healthcare. Global Advances in Health and Medicine 2: 38-57.
- Ziaka D, Tigani X, Kanaka-Gantenbein C, Alexopoulos EC (2025) A stress management and health coaching intervention to empower office employees to better control daily stressors and adopt healthy routines: A pilot randomized controlled trial. International Journal of Environmental Research and Public Health 22: 548.
- Ahmann E, Saviet M, Conboy L, Smith K, Iachini B, et al. (2023) Health and wellness coaching and sustained gains: A rapid systematic review. American Journal of Lifestyle Medicine 18: 162-180.
- Vargha A, Delaney HD (2000) A critique and improvement of the CL common language effect size statistics of McGraw and Wong. Journal of Educational and Behavioral Statistics 25: 101-132.
- Tomczak M, Tomczak E (2014) The need to report effect size estimates revisited: An overview of some recommended measures of effect size. Trends in Sport Sciences 21: 19-25.
Citation: Pipio A, Romano R, Sollami A, Marino A, Malagò G, et al. (2026) Impact assessment of structured health coaching intervention on perceived stress and sleep quality. HSOA J Psychiatry Depress Anxiety 12: 065.
Copyright: © 2026 Pipio A, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.

