
Monocular Diplopia Associated with Peripheral Iridotomy
*Corresponding Author(s):
Sailaja BondalapatiDepartment Of Ophthalmology, Atrium Health Wake Forest Baptist University, 177 Parkwood Drive, Elkin, North Carolina, 26821, United States
Tel:+1 9195239383,
Email:bondalapati29@gmail.com
Abstract
Laser iridotomy is the procedure of choice for primary angle-closure glaucoma. Ms. CS, a 47-year-old Caucasian female with a history of migraines, came to the clinic for an increased frequency of intermittent headaches, halos, and blurry vision in both eyes. Gonioscopy was performed in both eyes to assess the angles. The superior angles appear to be closed in both eyes with bare visualization of the posterior trabecular meshwork in the inferior/nasal and temporal quadrants. A plan was outlined to perform YAG Peripheral Iridotomy in both eyes to open the angles and then dilate the eyes on the return visit for a complete eye exam. The patient tolerated the procedure well but returned with monocular diplopia. Neurological pathways were assessed, and cortical pathology was ruled out. Cover-uncover test confirmed monocular diplopia with the right eye open. The patient's subjective symptoms were resolved when the iridotomy was covered with the eyelid manually. A neuro-ophthalmology consultation was pursued and confirmed the diagnosis of visual phenomenon from Laser Peripheral Iridotomy (LPI) causing monocular diplopia. The authors suggest corneal tattooing as a possible consideration to help resolve monocular diplopia, also may suggest considering superior locations, between 11'O-clock and 1'O-clock for laser in younger patients with no signs of dermatochalasis.
Keywords
Monocular Diplopia; YAG peripheral iridotomy; LPI; Migraines; Blurry vision; Narrow angles
Introduction
Glaucoma is the most common optic neuropathy, often outlined by damage to the optic nerve, a body that is vital to the transmission of messages between the brain and the eye. Progression is slow and is often first diagnosed when optic nerve changes are noticed in the long run. Onset is created when aqueous humor, builds up and is unable to drain through the trabecular meshwork efficiently. As pressure increases, the optic nerve gets progressively damaged, creating visual field deficits. This study focuses on Angle-Closure Glaucoma, categorized by severe headaches, eye pain, nausea/vomiting, blurred vision, halos around lights, and eye redness [1]. In this type of Glaucoma, occasionally, the iris bulges partially and completely block the angle. Risk factors include high intraocular pressure, age above 55, family history of glaucoma, migraine, high blood pressure, thin corneas, extreme hyperopia or presbyopia, chronic use of eye drops, and narrow drainage angle [1]. Treatment includes escalation therapy starting with multiple eye drops to laser treatments such as iridotomy, trabeculotomy, trabeculoplasty, to cataract surgery and tube shunt devices. For this specific study, we are focusing on the laser procedure called a YAG Peripheral iridotomy, which creates an opening in the peripheral iris for the additional drainage of aqueous humor, decreasing pressure and consequently reducing the risk of optic nerve damage. Adverse effects do exist; however, they are limited in number and lasting effects.
Case Report
Ms. CS is a 47-year-old Caucasian female with a history of migraines and heartburn. She came to the clinic for an increased frequency of headaches and blurry vision in both eyes (OU). She has a maternal family history of Glaucoma.
On presentation, the Best Corrected Visual Acuity (BCVA) with glasses was 20/20, Intraocular Pressure (IOP) was 24 OD and 25 OS and angles appeared to be narrow on the slit lamp exam. Hence, gonioscopy was performed in both eyes to assess the angles. The superior angles appear to be closed in both eyes with bare visualization of the posterior trabecular meshwork in the inferior/ nasal and temporal quadrants. A plan was outlined to perform YAG PI in both eyes to open the angles and then dilate the eyes on the return visit for a complete eye exam. YAG PI was placed at 10 O'clock (Figure 1) in the right eye and 2 O'clock (Figure 2) in the left eye. She tolerated the procedure well and the patient was sent home with prescribed steroid use for one week. On the return visit, the angles were moderately open to 30 degrees and headaches were relieved but patients started complaining of blurry vision with occasional twitches and flashes such as visual phenomenon. A complete dilated exam was performed to rule out retinal tears and detachment. Offered reassurance and discharged home with a plan for follow up in 3 months.
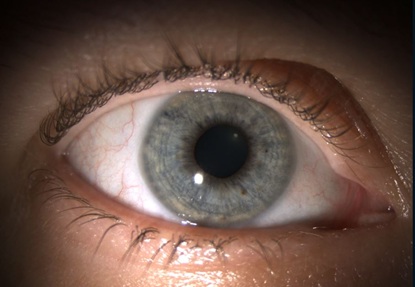 Figure 1: Right eye with LPI at 10 O’clock.
Figure 1: Right eye with LPI at 10 O’clock.
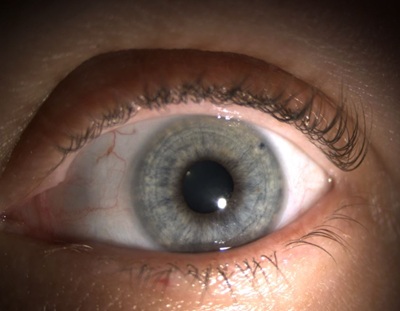 Figure 2: Left eye with LPI at 2 O’clock.
Figure 2: Left eye with LPI at 2 O’clock.
Patient returned back complaining worsening discomfort with ghost images and blurred vision with both eyes open. On exam, her BCVA was 20/25 with normal IOP and patent LPI. Her extraocular motility was full, and she was orthophoric. Cover-uncover test resulted in no phoria or tropia, but the patient reported monocular diplopia with the right eye open. Also, the patient felt comfortable with closing the right eye. Retinal pathology was ruled out and neuro ophthalmology consultation was pursued and confirmed the diagnosis of visual phenomenon from patent LPI causing monocular diplopia. Case was discussed with a cornea specialist and possible solutions of selectively opaque contact lens or corneal tattooing were offered to the patient. Patient agreed for a corneal tattoo (Figure 3) and the procedure was performed. She was happy on post operative day 1 with resolution of all her symptoms.
 Figure 3: Right eye with corneal tattoo covering the LPI.
Figure 3: Right eye with corneal tattoo covering the LPI.
Discussion/Conclusion
Monocular diplopia is defined as perception of overt double images, "ghost, shadow, or haze that persists when viewing with only one eye. Usually, monocular diplopia strongly supports an ocular cause such as refractive error, polyopia, dry eyes, cataract, or macular disease [2]. The diagnosis can be confirmed using a pinhole occluder over the viewing eye. In this case, the patient's subjective symptoms were resolved when the iridotomy was covered with the eyelid manually. Other differential diagnoses such as irregular astigmatism, dry eye and ocular pathology were ruled out using streak retinoscopy, fluorescein stain and macular OCT respectively. Reassurance was offered to the patient that the symptoms do not harbor any neurologic pathology as the diplopia was not binocular.
The literature is limited and very case specific on the complications of LPI. Among the complications, the most reported are bluish colored lines arising in thirteen patients assessed by Paul H. Murphy and colleagues [3]. When examining, each eye had an iridotomy partially exposed by the upper lid. When partially exposed, light traveling through the extra hole caused refractive error. Interestingly, symptoms completely disappeared when the iridotomy was fully open or closed. Due to dermatochalasis, older patients do not experience this complication as their skin becomes saggy, covering the hole. When the iridotomy is completely open, light travels uniformly through the iridotomy and passes onto the outer ring of the lens, which is often clouded due to cataracts. Therefore, the light is correctly refracted as the vision is not compromised [3]. Tognetto et.al reported a similar age patient (45), with Iris-Fixated Phakic Intraocular Lens (IFPIOL) in her left eye, underwent prophylactic LPIs, complaining of glare and photophobia [4].
After examination, her visual acuity was 20/20, pressure 14 mmHg and Iridotomies were preserved on the right and left eye (10 and 2 o’clock respectively), partially covered by the upper lid. Likewise, Ms. CS was happy with resolution of symptoms after covering her LPI in the right eye with corneal tattoo
The purpose of this paper is to review the complications of LPI and address corneal tattooing as a possible consideration to help resolve monocular diplopia. Also, may suggest considering superior locations, between 11'O clock and 1'O clock, for LPI in younger population with no dermatochalasis, and add more data to the literature. Although suture iridotomies and opaque contact lenses were addressed in the literature, corneal tattooing is less invasive than iris suturing and less cumbersome than maintaining a daily contact lens which involves a small risk of corneal infections.
Acknowledgement
Dr. Timothy Martin, Ophthalmology, Atrium Health Wake Forest Baptist University, Winston-Salem, North Carolina, United States
Statement of Ethics
Published research comply with the guidelines for human studies and the research was conducted ethically in accordance with the Declaration of Helsinki.
This retrospective review of patient data did not require ethical approval in accordance with local/ national guidelines.
Subjects have given written informed consent to publish this case (including publication of images). All patients are referred to by aliases, rather than their real name.
Conflict of Interest
The authors have no conflicts of interest to declare.
Funding Sources
The authors have no sponsors to declare.
Author Contributions
Ghatti, Suhas was responsible for the literature review and analysis of the case report. He researched similar cases and treatments, identified unique aspects of the case, and discussed the implications of this for future research or clinical practice. He was also responsible for reviewing and editing the case report to ensure that it was accurate, clear, and well-supported by the literature.
Bondalapati, Sailaja was responsible for case presentation and data collection. She is a primary physician involved in the patient’s care, providing the patient's medical history, presenting symptoms, and running diagnostic tests. She was also responsible for obtaining the patient’s consent to publish the case report.
Data Availability Statement
Data Available at Wake Forest Ophthalmology Clinic at Elkins, North Carolina
References
- Mayo Clinic. Glaucoma, Mayo Clinic, USA.
- Glisson CC (2019) Approach to Diplopia. Continuum (Minneap Minn) (Neuro-Ophthalmology) 25: 1362-1375.
- Murphy PH, Trope GE (1991) Monocular blurring. A complication of YAG laser iridotomy. Ophthalmology 98: 1539-1542.
- Tognetto D, De Giacinto C, Cirigliano G (2017) Suture of Symptomatic YAG Laser Peripheral Iridotomies Following Phakic Intraocular Lens Implantation. J Glaucoma 26: 675-677.
Citation: Ghatti S, Bondalapati S (2023) Monocular Diplopia Associated with Peripheral Iridotomy. J Ophthalmic Clin Res 10: 111.
Copyright: © 2023 Suhas Ghatti, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.

